Exclusive:NHS Scotland winter crisis: 24-hour waits, patients lying in corridors, and staff ready to quit - A&E doctor on why 'code black' alert now 'pointless'
An accident-and-emergency (A&E) doctor has said hospitals declaring a ‘code black’ emergency would now be “pointless” – due to emergency departments already being at breaking point across Scotland and there being no room for escalation.
Dr Lailah Peel, an A&E medic working in the Central Belt, told The Scotsman that pressures in NHS Scotland’s emergency departments had left staff “wondering how much more they can take”, with the only “good days” coming when doctors feel they “are not running around thinking someone is going to die”.
Advertisement
Hide AdAdvertisement
Hide AdPatients are already being left waiting outside in ambulances, which does not count towards Scottish Government A&E waiting times figures, and sick people are being dumped in corridors “with no real nursing or medical care” while they wait to be seen, the medic claimed.
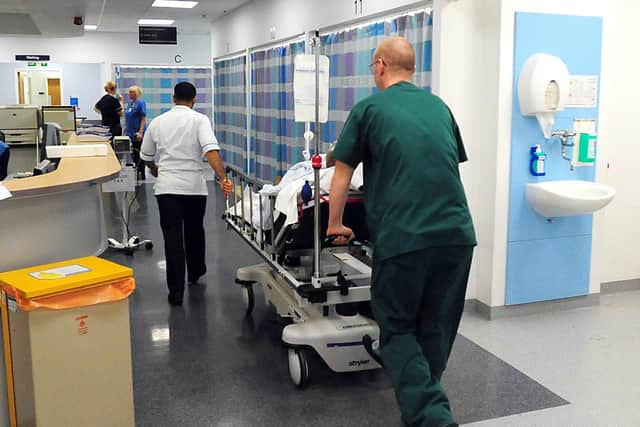

Dr Peel also said 24-hour waits were “no longer unusual” in Scotland’s A&E departments, with some managers even admitting “they hope people just don’t turn up”. The claim has been backed up by the recent revelation that 4,000 Scots waited more than 24 hours in A&E in the first six months of this year.
And it comes as NHS Lanarkshire yesterday urged people to either call NHS 24 or 111, saying its emergency departments within University Hospitals Monklands, Hairmyres and Wishaw were “extremely busy”.
Asked whether health boards were considering declaring a ‘code black’, meaning hospitals are full and can only treat the most severe cases, Dr Peel said: “It would be pointless because there isn’t much room for escalation. One of the really frustrating things is, I was on at the weekend, and both days I came in to patients on 15-hour bed waits.
“When staff tried to escalate it, and ask ‘what’s the plan?', a manager said they hoped people just don’t turn up.”


Asked how today’s conditions in emergency departments compare with the winter crisis earlier this year, Dr Peel said: “It’s the same as last winter. We saw some improvements over the summer, but realistically I don’t think we’ve seen a huge amount of change. It’s hard to measure – it’s just anecdotal.
“Our baseline is totally skewed. When we’re not running around thinking someone is going to die, that’s a good day. We have increasing pressure, wards shutting down due to Covid outbreaks, while staffing is terrible everywhere.
“We’re all looking at each other and wondering ‘how much more can we take?’”
Advertisement
Hide AdAdvertisement
Hide AdThe proportion of patients waiting 12 hours or more in A&E is at the highest level since January, new figures have shown.


In the week up to October 29, 6.6 per cent (1,644 people) of those attending Scotland’s emergency departments waited half a day or more, up from 5.7 per cent the previous week. The last time this figure was as high, according to Public Health Scotland, was during January’s winter crisis, when it was 7 per cent.
The Scottish Government aims to ensure 95 per cent of patients are seen within four hours.
On the A&E statistics, Dr Peel, who chairs the British Medical Association Scotland’s LNC forum, said: “It’s not unusual to see people going beyond 24 hours now. I’m seeing a lot in the 12 to 24-hour window.
“What we’re not getting is patients being booked in while waiting in ambulances. There’s waits every step of the way.


“I’ve seen patients deteriorating over that time. Most people are stable, theoretically, during the wait, but I’ve seen patients waiting for intensive care and high dependency beds. I’ve heard people come into A&E with a broken hip, then go to surgery straight from the waiting room.
“There have been people waiting outside in ambulances, whereas other departments will take them off and put them in a corridor.”
The Royal College of Emergency Medicine Scotland’s vice-president, Dr John-Paul Loughrey, said the college was “concerned” the Scottish Government’s winter plan “fell short of delivering what is needed ahead of what will likely be a difficult period for emergency care”.
Advertisement
Hide AdAdvertisement
Hide Ad“We desperately need to see an increase in bed numbers,” he said. “This will help to reduce the dangerously high levels of bed occupancy, reduce long and dangerous delays in A&Es, and help to ensure patients are admitted to a bed more promptly.
“We continue to engage with the Cabinet secretary and his team in good faith and raise the concerns of our members. To avoid what could be a devastating winter, we again urge the Scottish Government to heed our calls to adopt our priorities to resuscitate emergency care.”
Health secretary Michael Matheson said he was “clear that A&E performance is not where it needs to be” and that he would “continue to work closely with [health] boards to support delivery of sustained improvements”.
“Monthly figures for September show a slight decrease in four-hour performance, which is consistent with monthly trends seen in previous years, with England also seeing a decrease in performance for this period,” he said.
“We know that long waits remain too high. However, patients experiencing the longest waits will generally be those who require admission and are waiting on a bed in a ward. These patients will have been triaged and seen by a doctor prior to decision to admit.
“Scotland’s core A&E departments remain the best performing in the UK. Our winter plan will support boards to maximise capacity to meet demand and our £12 million expansion of Hospital at Home will ensure people receive care at home or as close to home as possible, where clinically appropriate, to help reduce pressure on our emergency departments.”
Comments
Want to join the conversation? Please or to comment on this article.