Covid Scotand: Protect NHS to avoid collapse like northern Italy in 2020, top medic warns
Mike McKirdy, president of the Royal College of Physicians and Surgeons of Glasgow (RCPSG), said if the NHS is overwhelmed in the new year, Scotland may face a scenario like that already seen in Northern Italy in April last year, as well as in New York and India at earlier stages of the pandemic.
These crisis situations saw reports of doctors being forced to choose which patients to save, due to equipment, bed and staffing shortages. Mass graves were also used in New York and Italy.
Advertisement
Hide AdAdvertisement
Hide AdIt comes after Nicola Sturgeon warned the new variant may achieve “what we have feared all along” in overwhelming the NHS.
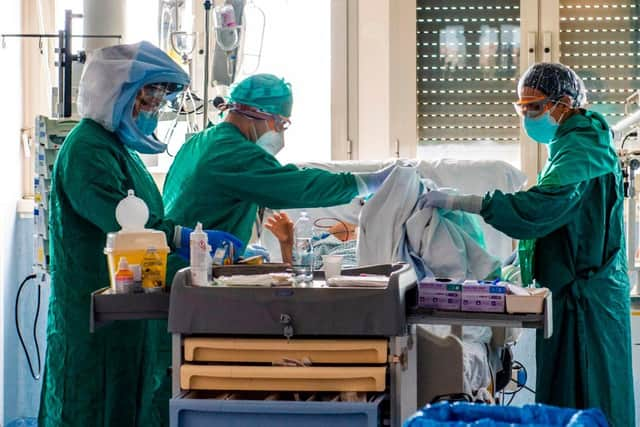

Dr David Shackles, joint chair of the Royal College of GPs in Scotland, said the threat from Omicron “cannot be overstated”, and there is “palpable concern” for the health service.
Health boards said they are facing continued pressure over high demand and staffing shortages, as NHS Greater Glasgow and Clyde banned all, but essential hospital visits for patients in shared wards over the risk of Omicron.
Mr McKirdy said he was not predicting that a crisis on the scale of that in Northern Italy would happen in Scotland, but that this is what the country is at risk of.
“We should all be worried about the potential impact,” he said.


He asked members of the public to follow politicians’ advice to reduce social mixing, thereby reducing infections.
“Lots of infections will become lots of ill people, and lots of ill people have the potential, depending on how serious this variant is in terms of the illness it causes, to overwhelm the NHS,” he said.
NHS Greater Glasgow and Clyde (NHSGGC) has said from Monday patients in shared wards will not be allowed visitors, apart from essential visits such as those for mental health reasons or end-of-life care.
Advertisement
Hide AdAdvertisement
Hide AdPatients in single rooms will be allowed one visitor a day, while children and those in maternity wards will be allowed two.
Jennifer Rodgers, deputy nurse director at NHSGGC, said the decision to restrict visiting had been “difficult” and would be applied compassionately.
“I am truly sorry that it is necessary to change our visiting arrangements and I fully understand the impact that this will have on our patients and their families,” added deputy nurse director Angela O’Neill.
NHS Lothian said the health board continued to be under “extreme and sustained pressure” and asked members of the public to call 111 before visiting accident-and-emergency unless it was critical.
Jacquie Campbell, chief officer of acute services at NHS Lothian, said: Our services continue to be under extreme and sustained pressure due to a combination of staffing and bed pressures, combined with high volumes of patients presenting with complex and serious cases.”
Dr Shackles said he was concerned about the impact of Omicron on general practice, which is already operating “well beyond” capacity.
“Like the rest of the health service, GPs and their teams are currently putting plans and systems in place to do all they can to ensure that patients can continue to access GP care over this challenging period,” he said.
In some cases, GPs have had to refuse requests to help with the booster vaccination campaign because of pressure on their own services, Dr Shackles said.
Advertisement
Hide AdAdvertisement
Hide Ad"For many practices this simply won’t be possible as there is currently no extra workforce capacity across general practice and releasing staff for the vaccination programme may mean that GPs wouldn’t be able to provide care safely to patients,” he said.
While there is not enough data about the effect of Omicron yet, Mr McKirdy said leaders already know what overwhelming the NHS might look like, having seen similar situations in other countries.
“We saw it in New York, we saw it Italy, we saw it in India, we’ve seen it in France,” he said.
“Nobody wants that to happen. Therefore, we're putting plans rapidly in place in terms of facilities and staffing, but … that’s a really big challenge, and this is going to hit us at the most difficult time of year.”
January is the worst time of year to be facing a new variant, Mr McKirdy said, as public holidays as well as increased travelling to see loved ones will likely increase spread.
He pointed to the January of 2000, which saw a spike in flu cases that caused the NHS to “nearly fall apart”.
“I think there's a moment here to look back to the very beginning of this, in March/April 2020, when we watched on our television screens the health service in New York dismantle, and we watched the health service in the north of Italy fail to cope,” he said.
“That meant literally in New York there were mass graves, and in Italy there were, in effect, mass graves.
Advertisement
Hide AdAdvertisement
Hide Ad“I’m not saying that’s going to happen … but what we all know is that there have been examples from all over the world.
“We know earlier this year, when the Delta wave went through India we were familiar on our television screens with watching people in hospital car parks trying to have oxygen delivered through their relatives getting an oxygen tank or an oxygen mask.”
Mr McKirdy said is is confident the NHS will “rise and to try and meet the challenge”.
But he added: “The NHS is going to have its facilities tested, and it's going to have its workforce tested, at a time when both of these resources have been through a pretty challenging 21 months already.”
A message from the Editor:
Thank you for reading this article. We're more reliant on your support than ever as the shift in consumer habits brought about by coronavirus impacts our advertisers.
If you haven't already, please consider supporting our trusted, fact-checked journalism by taking out a digital subscription.
Comments
Want to join the conversation? Please or to comment on this article.
