Insight: 'I am not watching Blue Planet, but the removal of a healthy organ for transplant'
It is a mesmerising scene; so mesmerising I have to stop and remind myself what is happening here. The image on the screen is not some underwater ecosystem but the insides of my friend and colleague Cat Thomson, who is lying, anaesthetised, on the bed in front of me. And I am not watching an episode of David Attenborough’s Blue Planet, but the removal of a healthy organ for transplant.
Cat, 51, who lives in the Borders, has promised her left kidney - which she has nicknamed Sidney - to her older sister Jenny Crossley, 53, in Wales. This morning it is being extracted in operating theatre number 14 in Edinburgh Royal Infirmary (ERI). And this afternoon it will be flown more than 300 miles to be implanted in Jenny.
Advertisement
Hide AdAdvertisement
Hide AdBecause Cat, Scotland on Sunday’s picture editor, wants to encourage more living donors, she is allowing photographer John Devlin and me to follow every step of that journey.
I have already written about the sisters’ relationship; about Jenny’s polycystic kidney disease and the deterioration in her condition which has left her in need of dialysis and a transplant. I have written about the lengthy assessment process Cat undertook to ensure her blood and tissue match were compatible with her sister's and that she was healthy enough to undergo the operation.
Now I am being given a ringside seat as consultant transplant surgeon Andrew Sutherland performs hand-assisted laparoscopic keyhole surgery on someone I have worked with for years.
Our day had started at 8am when John and I visited Cat in Ward 215 - the ERI’s High Dependency Unit. She set aside the book she was reading - Michelle Obama's memoir, Becoming - and stoically flaunted her gown and compression socks. The sisters had already exchanged texts. “Jenny just wrote: ‘I don’t know what to say,’” Cat told us, "and I replied: ‘You don’t have to say anything’.”

We accompanied her as she was wheeled in her bed to the lift, then ran down the stairs so we could wave her off at the doors of the hospital’s theatre suite. Covid restrictions meant we could not be with her as she was intubated, so we did not see her catheter fitted or the cannulas for fluids and anaesthetic inserted in her arms.
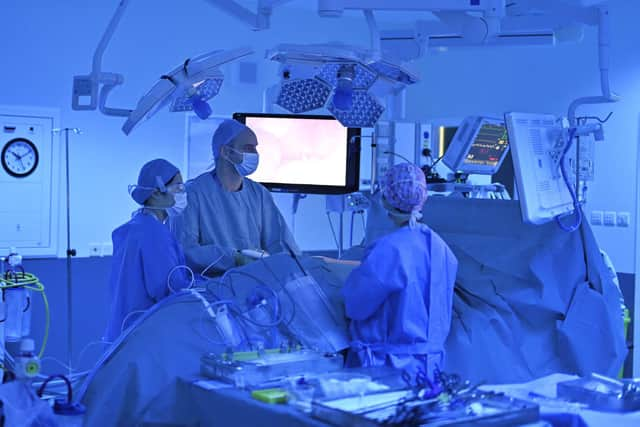
But at around 9.30am, we changed into scrubs and entered the operating theatre. It was surprisingly cool and airy. Cat had been positioned on her right side and covered with green drapes so only a small part of her abdomen was exposed. Around the operating table were Sutherland, his surgical assistant, an anaesthetist, a scrub nurse, two other nurses and a clinical support worker. Living donor transplant coordinators Nina Kunkel and Sarah Lundie were also in the room.
Dozens of transplant operations have already been carried out in the ERI this year. Sutherland had performed a removal (nephrectomy) the day before. And today, in the operating theatre next door, another surgeon was preparing to implant a kidney from a deceased donor into someone on the waiting list. But kidneys from live donors start more quickly and tend to last for longer.
By the time we arrived, Sutherland had already made the first of three cuts in Cat’s stomach - an 8cm slit containing a rubber cylinder through which he had inserted his gloved left hand. Now we are watching him make two smaller incisions: one for the surgical instruments, the other for the laparoscopic camera which captures the internal images and relays them to the screens.
Advertisement
Hide AdAdvertisement
Hide Ad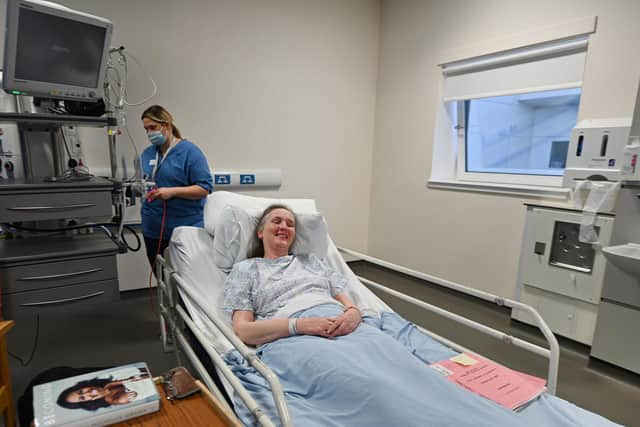

At the shout of “gas on”, carbon dioxide is pumped in to inflate Cat’s abdomen and create a bigger operating space inside her. Then Sutherland guides the instruments through that space, cutting tissue, dislodging the spleen and the colon, as he makes his way towards our colleague’s kidney. It is, John and I agree, an unsettling, but remarkable spectacle.
**********
I had first met Sutherland the previous afternoon when he was briefing Cat on the ins and outs of the procedure. She had been admitted to Ward 215 earlier that morning and endured more blood tests and an ECG. She had been poked and prodded and asked again what she wanted doctors to do with her kidney in the extremely unlikely eventuality that - having been removed - it could not be implanted in Jenny. The options were: reimplant it, give it to research, give it to the next person on the waiting list or discard it. "Don't throw it in the bin," Cat yelped.
When the surgeon handed her the form, she ticked "give it to the next person on the waiting list" box. She said once she had made the decision to donate, she would have gone ahead regardless of the beneficiary. But ticking that box means that, should Cat’s kidney be diverted to someone else, Jenny would be prioritised on the waiting list to receive the next available kidney.

Sutherland has been a consultant transplant surgeon since 2016. A mountaineer who once climbed Everest, he has a particular interest in how both climbers in high altitudes and extracted organs cope with reduced oxygen.
He explained CT scans had helped him understand Cat's anatomy. He knows the kidney he will remove has two arteries, so there will be no surprises there. But the scans couldn't tell him everything. “It’s like having a map with only the motorways and A roads on,” he said, “but the reality is there are all these other trunk and minor roads you can’t see on the map, so you have to feel your way through the operation and deal with what you get when you are there.”
The aim is to clear the tissue from around the kidney and surrounding tubes and vessels, then detach it from the abdominal wall until it is hanging by only its arteries, vein, ureter (the tube that connects it to the bladder) and the gonadal vein. Sutherland will then dissect and clip the ureter and gonadal vein before firing two lines of staples along the vein and the arteries, dissecting between the staples.
As the first of Cat’s arteries is stapled, a digital clock will start counting the seconds until the kidney is perfused - flushed through with a sterile fluid called Soltran - and chilled to four degrees centigrade.
This is important because, with its blood supply now cut off, the kidney is receiving no oxygen. Cooling it reduces the oxygen requirement of the cells. But if starting the perfusion takes too long, there may be cell damage.
Advertisement
Hide AdAdvertisement
Hide AdInitially, the operation is slow and the body parts difficult to decipher. The first time Sutherland points out the gonadal vein I nod obligingly, but all I really see is a throbbing mush. However, as the instruments - a harmonic scalpel, with secateur-like blades, and a diathermy, which hooks and pulls - remove the tissue and fat, its shape becomes clear. It looks like a long pink worm.

The instruments cut through small blood vessels too, cauterising as they go. Sometimes the bleeding is enough to require swabs, which are counted in, and will be counted back out, before Cat’s wounds are stitched.
After an hour or so, John and I give the theatre staff a break. We stay away for a short stressful period when Sutherland is dividing lumbar vessels near the arteries.
By the time we return, at 12.20pm, the kidney has been detached from the abdomen wall. There’s a brief lull - long enough for me to wonder at it dangling in space - and then everything seems to happen at once. The gonadal vein and ureter are disconnected and clipped. Then the staple gun appears, and rows of 1mm titanium clips are fired at the renal vein, and then the arteries, one after the other.
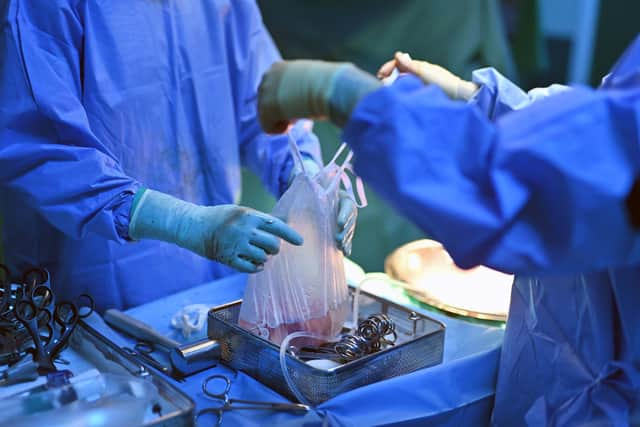
I know the first artery has been stapled because someone shouts “start clock,” and the red digits on the far wall begin to turn: 0.01/0.02/0.03. Cat’s kidney is pulled through the hand-port incision and placed in a bowl for perfusion.
For a brief period, it’s like a premature baby has been born. All attention shifts from Cat to the fragile five-inch parcel that has emerged from her body. Heads are bent over the bowl as the staples are cut off and a long cannula is inserted in the artery.
As the Soltran is flushed through, the blood - at first scarlet - turns a pinker shade of pale, and then runs clear, while the kidney - at first pink - blanches grey-ish. At some point, I look up and see the clock has stopped at 3 minutes 31 seconds. Later, Sutherland will explain the more important time - the "warm ischaemia time" - which is the time from the second artery clamp, when the blood supply stops, to perfusion - was 2 minutes 46 seconds which he says is very good.
Right now, though, it’s still all hands on deck. The surgeon is with Cat, checking for bleeding and that all the swabs have been removed. He can't find the red band that had been tied round one of the arteries, and calls to the scrub nurse who locates it in the bowl.
Advertisement
Hide AdAdvertisement
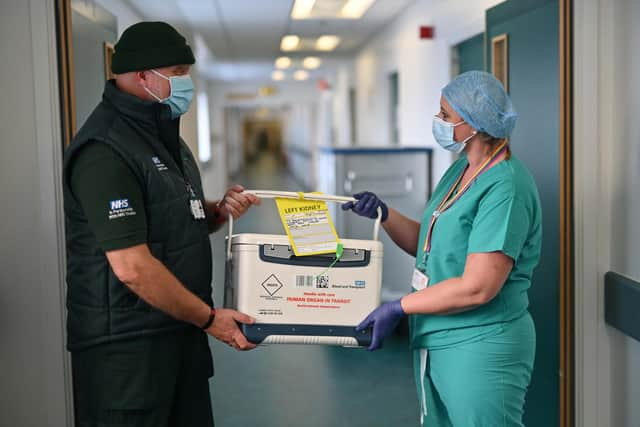
Hide AdShe has been trimming the fat to reveal the smooth wet pebble of a kidney below. Trimming the fat helps it cool. But preparing the kidney for implantation is the job of Jenny’s surgical team in Cardiff, so soon the nurse is triple bagging it and placing it in the ice box, marked Human Organ in Transit.
Kunkel, meanwhile, has been recording details, such as the length of the arteries, and gathering vital documents ready for transportation. She lays the folder on top of the ice. The box is sealed and a tag attached. It's a yellow tag for Cat’s left kidney; right kidneys get a red tag.
Though kidneys last longer than other organs, time is of the essence. John and I shout “good luck” to the still unconscious Cat, take off our scrubs and emerge on the other side of the changing rooms to find a courier - Jock Atkinson - waiting.
Atkinson works for IMT Medical Transport which coordinates the transportation of organs across the country. Ex-military police, he landed the job after a soldier he served with in Belfast put him in touch with the company. Once in the ambulance car, he takes a photograph of the kidney box to send to control then sets off, bemoaning the fact that, in Scotland, he cannot use his blue light without specific authorisation.
Today, though, the traffic is light. At Edinburgh Airport, we clear security at Signature Flight Support in minutes and before I know it I am boarding a private Learjet 45 with the precious cargo.
We soar into a sun-split winter sky. As the jet ploughs its way towards Wales and Jenny, I gaze on the billowing clouds, with their ridges and furrows, cavities and crevices. Through the cracks, I can see motorways, A roads and country lanes, pulsing like veins and arteries, and I think, again, of the quotidian miracle I have witnessed.
When we land at 3pm, I switch my phone back on and Cat has already texted. “All OK," her message reads. "Back in the ward. Bit sore. Not too bad. Music playing. Together in Electric Dreams.”
***********
At Cardiff Airport, Cat’s kidney is met by courier James Baker. It’s afternoon now, and the traffic is heavier. It takes almost an hour to battle through it. We arrive at the University Hospital of Wales at 4pm and walk to the theatre suite together. The Covid restrictions are tighter here so I am not - as originally planned - allowed to watch the implantation. This time it’s my turn to text. I send Cat a picture of Baker and write: “Sidney on his way to Jenny.” She sends me back a smiley face.
Advertisement
Hide AdAdvertisement
Hide AdLater, Jenny’s surgeon Laszlo Szabo, fills me in on what happened next. “When the kidney arrived we had to clean the arteries and the vein, “ he says. “There’s always some extra fat we have to remove. So we prepared the kidney for transplantation, and then around 4.15pm, we sent for the patient.”
The kidney implantation is open rather than keyhole surgery. The surgeon does not remove one of the diseased kidneys to make space for the new one. Instead, he places it at the lower abdomen where the ureter can be connected to the bladder and the vein and arteries to the iliac vessels which run down into the leg.
When a donor kidney has more than one artery, the surgeon has a choice: he can join them together on the backbench when he is preparing the organ for transplant and do a single anastomosis (join) to the recipient vessels. Or he can do two separate anastomoses.
In Cat/Jenny’s case, Szabo explains, the arteries were too far apart to be easily connected to each other, so he joined the vein first, then the two arteries separately.
Just as the kidney blanches when it is perfused with Soltran, so it turns pink again when it is reperfused with blood. Everyone talks about that moment when the arteries are connected and the clamps removed, and the colour returns. I imagine it like a lightbulb being switched on and wish I could view it for myself. Szabo sees it often. “But it’s amazing every time.” he says. After the vessels were joined and the kidney reperfused, he joined the ureter to the bladder.
I stay over in Cardiff and the following morning, Jenny says I can visit. It’s a privilege because her husband Martin, who teaches maths and engineering students, has not been allowed in. Like all transplant patients, Jenny is on immunosuppressants to stop her body rejecting the new organ. These powerful drugs make her vulnerable to infection. But I’ve spent the days before the transplant self-isolating and taken five days’ worth of lateral flow tests, so the ward manager says I can grab a few minutes. I put on gloves, an apron and surgical mask and go in.
It’s great to see Jenny, whom I have previously only spoken to by phone. She is sitting up in bed but looks tired. On hourly observations, she has been unable to get any sleep. “I did drop off for a minute but then I woke with a snore into my oxygen mask,” she says. Her cramps have stopped, but her blood pressure is too high and her heart has been racing. This is unexpected and cardiologists are trying to find out why. She’s clearly anxious, so I say goodbye and head out of the hospital.
That was nine days ago. So, what has been happening since? When John visited Cat, hours after her nephrectomy, she said she felt she’d been hit by a small bus rather than the big bus the live donor kidney team had forecast. For 24 hours, she had a pain relief pump which released analgesics every five minutes. The following day, her catheter was removed and she moved from her bed to the chair.
Advertisement
Hide AdAdvertisement
Hide AdBut Saturday was tough. The gas pumped into Cat's stomach made her constipated and caused her to be sick. Doctors decided to insert a nasogastric tube to decompress the stomach, rest the bowel and drain any excess to stop her vomiting. The tube was unpleasant and delayed her release.
“I’m not ashamed to admit I cried,” she says. But she got home last Sunday night, and hasn’t looked back. She has already been for five-minute walks in the fields around her house. Before she left hospital, her creatinine level (a measure of how well kidneys are filtering waste from your blood) was back to normal levels even for someone with two kidneys. “I mean that’s mind-blowing,” Cat says.
She is concerned for her sister though. Sidney is performing well. At some points, Jenny’s kidney function has been close to normal (up from single percentage figures at her most ill) but the issues with her heart have continued.
At first cardiologists feared she had suffered a small heart attack, but an angiogram on Monday showed no blockages to the arteries. Now they believe she is suffering from takotsubo cardiomyopathy: a temporary weakening of the heart caused by physical and/or emotional stress. “They say if you treat it with drugs to slow the heart down gradually it usually resolves itself within a few weeks,” Jenny says.
Her kidney function has been fluctuating as a result of the drugs being used to treat her heart and she is finding it difficult to eat solids, which has left her weak. “I can get from the bed to the chair and back again, but that’s about all.”
Martin is still not able to visit and she did not make it home, as hoped, for her daughter’s birthday yesterday (Saturday). On the plus side, the end of her low-potassium diet means she had her first hot chocolate for a long time. “It’s a question of being patient,” she says. “And I’m so relieved Cat is doing well.”
As for Cat, she has no regrets. “It’s completely unreal. I’m very glad I could do it,” she says. “You think of all the obstacles that could be in the way of it happening - yet it did happen."
Before the operation, Jenny could only walk a couple of blocks. “I hope the next time I see her she is full of joy and energy,” Cat says. “I don’t think there’s anything you could do that’s quite so measurable in terms of improving someone’s life and I’ve eased the worries of my wider family too.”
Advertisement
Hide AdAdvertisement
Hide AdShe ends the call by saying if she had more kidneys to donate, she would. I leave her to her Michelle Obama book. Although I reckon, as inspirational figures go, she could give the former First Lady a run for her money.
Scotland on Sunday will revisit Cat and Jenny soon to find out how their recovery is going. In the meantime, we are grateful to NHS Lothian, NHS Wales and IMT Medical Transport for the unprecedented access and cooperation.
Comments
Want to join the conversation? Please or to comment on this article.
