Health anxiety: Why the crisis in NHS Scotland's GP services is leading to more patients using 'Dr Google'
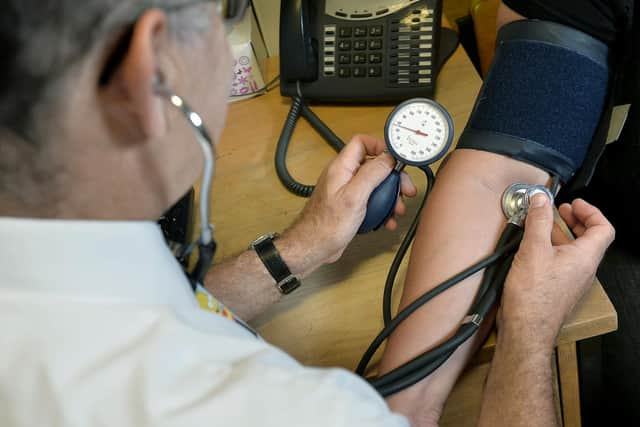
Packed GP waiting rooms, increasing diagnostic referral times and a retention crisis in Scotland’s primary care system is creating a vacuum of information for patients distressed by their symptoms – a gap the internet is happy to fill.
Searching for symptoms online, or ‘Dr Google’ as it colloquially known, can cause a great deal of anxiety for patients, due to the large number of alarming articles which can be brought up by searching for common symptoms such as headaches or persistent coughs.
Advertisement
Hide AdAdvertisement
Hide AdThere are two main reasons for this. Firstly, there are countless websites dedicated to providing health information, using keywords found in common web searches, which exist purely to make money through ad revenue. The onus is on web traffic, not reliability.

Secondly, news articles often feature emotive stories of rare diseases, or young people suffering from diseases they otherwise would not be expected to develop. These stories make the news because of their rarity – a person in their 80s dying of cancer is a frequent occurrence, but a person in their 20s developing a terminal condition is incredibly rare.
However, this can lead some people to erroneously believe they are likely to be affected by any number of diseases highlighted in the media, when in fact the enormous rarity of the disease is the reason it was considered newsworthy in the first place.
The Scotsman spoke to Dr Andrew Buist, from the British Medical Association (BMA), and Dr Chris Williams, from the Royal College of General Practitioners (RCGP), to find out more about the pressures faced by GPs in Scotland, and where patients can go for reliable information.
Dr Buist, who chairs the BMA’s Scottish GPs committee, said: “Now, just pick up your smartphone and type in ‘brain cancer’ and you’ll find lots of websites telling you the symptoms and signs to look out for, and there's nothing we can do about that.
“We cannot put the internet back in its box. It’s an incredibly useful thing, we all use it everyday, but I think the important thing is for patients to be directed to what we call reliable sources of information.”
Dr Buist highlighted the NHS Inform website as a good example of easily accessible, measured information. “You will get reliable information there, rather than the more scrupulous places on the internet, where they may have a commercial angle, and it might be about selling something to you rather than giving you hard facts,” he said.
“I don't have a problem with patients using the internet and coming to me with the concerns, it has always happened, it just happens a bit more often though.”
Advertisement
Hide AdAdvertisement
Hide AdDr Williams said there were “two specific dangers” in terms of using internet search engines. “One of the dangers that I would highlight is that there are sponsored links on Google,” he said. “Google isn't just finding you information that is relevant to you, it's also presenting choices of website to you that you might not otherwise have taken.
“The other thing is that it can lead you to information that is quite emotive, that maybe tells about a very rare, unusual or less common things that might immediately get people worried – do they have cancer? Do they have something that needs a very different approach to testing?
“They might see things that then have them thinking several steps ahead in a process of diagnosis. One of the advantages of consulting with a GP, or another member of our clinical team, is being able to help people navigate their way through this, to be able to answer questions, not just to providing information.”
Dr Buist added: “I would add the media plays a huge factor in all of these sorts of things. The public don't worry about things they should be worried about, like alcohol, obesity, a lack of exercise and mental health, and worry about things they probably don’t need to.”
There is evidence that health anxiety, or hypochondriasis, has been on the rise following the birth of the internet, and the more recent coronavirus pandemic led to an increase in health anxiety and other mental health problems.
A literature review from 2023, of 33 different studies, found the results “suggest that social anxiety has been heightened in the general population due to the pandemic, with women and low-income earners being especially vulnerable”.
“Other contributing factors include impaired coping strategies, lower socio-emotional well-being, limited support networks, and contraction of the SARS-CoV-2 virus,” the authors said.
Sufferers or health anxiety can be consumed by their fear, which is not relieved by the assurances of doctors or diagnostic testing. Patients will avoid media that might mention their disease fixation, and may avoid physical exertion. The disorder can also lead to ‘phantom symptoms’, caused by anxiety, which are taken by the sufferer to be indicative of a different disease.
Advertisement
Hide AdAdvertisement
Hide AdFor example, patients may associate numbness or tingling on a patch of skin with a serious disease, and keep rubbing that area to check, in turn causing more numbness and tingling, ultimately creating a ‘feedback loop’ of anxiety that can result in a panic attack.
The root cause of the crisis in Scotland’s primary care, according to both Dr Buist and Dr Williams, is the retention of GPs.
Dr Williams said: “The job has changed over over the years, in terms of intensity of work, in terms of the number of clinical contacts during the normal working day, and also in terms of the complexity of the cases that we see.”
Doctors who are later in their careers “are reflecting on what the job used to be”, he added, and many are leaving the profession or scaling down their hours.
Comments
Want to join the conversation? Please or to comment on this article.