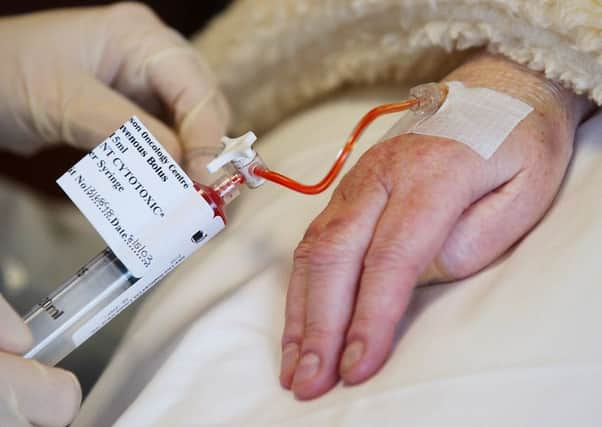
Woman having chemo for stage 4 cancer '˜not sick enough' for benefits

Neither did her doctors – it took 10 months for them to realise her persistent cough and itchiness were not just a chest infection and eczema.
The bakery worker had grown increasingly worried about her breathlessness – and by October last year had almost collapsed walking into her GP surgery.
Advertisement
Hide AdAdvertisement
Hide AdThen came the shocking news – she had stage 4 Hodgkin’s lymphoma, meaning it was advanced and had spread to her lymph nodes and lungs.
She also wasn’t prepared for just how sick and tired she would constantly feel when she endured four rounds of gruelling chemotherapy.
But Paige, from Flintshire, North Wales, says she not only had to deal with the stress of her illness – she also faced a battle to get financial help.
She explained she was left in tears after she discovered she’d been deemed “not sick enough” for disability benefit after a home assessment during the time she was having treatment.
“The assessor turned up about four days after my second to last chemo round,” she told i. “I was sat on the couch in my PJs with no hair. I was lethargic and my head felt so heavy I had to keep it rested on the sofa arm or physically hold it up with my hands.
“The letter said I was physically well enough to take care of myself and my mental health was fine – which she didn’t even ask me about.
“I cried, I felt like I’d been personally judged. It made me feel like a fraud, like it was my fault that I was ill.”
‘I was asked to stand on one leg’
Paige was advised by her CLIC Sargent social worker that she’d be entitled to Personal Independence Payment (PIP), a benefit that helps with the extra costs of living with a long-term health condition or disability.
Advertisement
Hide AdAdvertisement
Hide AdThe weekly rate for the daily living part is either £57.30 or £85.60 and for the mobility part, either £22.65 or £59.75.
Paige was hoping to have the money to pay for her travel costs for trips to the hospital three times a week. She says the questions she asked by the assessor were “too black and white”.
“Everything has to be a yes or no. She asked if I could prepare food by myself and I said yes, but not for the first week or so that I start a new cycle of chemo. But that was obviously taken to mean I don’t need any help.
“The report said I wasn’t lethargic, when I couldn’t lift my head off the sofa to speak to her it felt so heavy. It also said my mental health didn’t seem affected when I wasn’t even asked how I felt. Of course I’m affected by having stage 4 cancer. She didn’t listen to me at all.
“I was asked to stand on one leg, which I could do. What does that prove, I still have cancer. It’s ridiculous that they even wanted to see me to check my claim. Why isn’t my GP’s letter that I had cancer and was having chemotherapy proof enough?”
‘So de-humanising’
With her social worker’s help, Paige managed to successfully appeal the decision and was awarded PIP in May this year – around seven months after she had first been diagnosed with cancer.
“People with cancer need the financial help at the time they apply for it, when they’re off work sick and have extra costs to travel for treatment,” she said.
“The whole experience of PIP has been so negative and de-humanising. I was made to feel like I’m doing something wrong for being ill.”
Advertisement
Hide AdAdvertisement
Hide AdPaige finished her chemotherapy in March this year and a scan has shown she is cancer-free.
The Department of Work and Pensions spokesperson said: “We are committed to supporting people with disabilities and health conditions. We support 1.88 million people through PIP and 1.97 million people through DLA. We have never spent more on benefits for disabled people and people with long-term health conditions, totalling over £50bn a year – up £7bn since 2010. Under PIP, 30% of claimants receive the highest rate of support, compared with 15 per cent under DLA.
“But we constantly seek to improve the quality of PIP assessments. We have commissioned to independent reviews of PIP, and most recently announced that we will pilot video recording of assessments, improving confidence in the assessment process. We will continue to reassess the quality of the process to ensure that it works well for everyone.”
• This article first appeared in our sister publication, The i