Hospital ward switches put elderly lives ‘at risk’
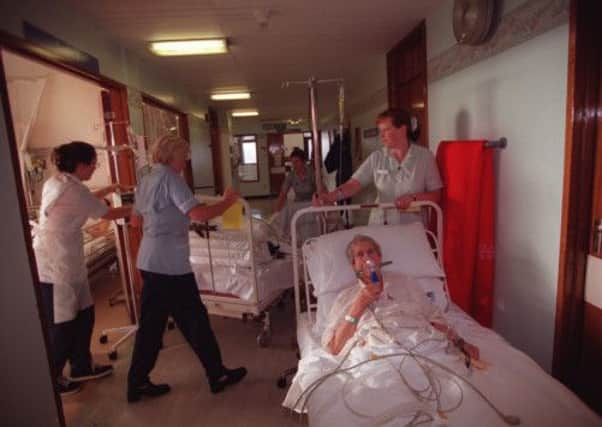

The practice of “boarding” – moving patients to wards outside their speciality in order to cope with new patients coming in – has become common in many hospitals as demand for services grows.
But experts from Dundee University have warned this growing trend is putting patients at risk, especially the oldest and most vulnerable.
Advertisement
Hide AdAdvertisement
Hide AdMedics and campaigners have also joined the growing disquiet about how a cut in the number of beds is affecting care, against a backdrop of increasing demand on hospitals.
Professor Marion McMurdo and Dr Miles Witham, from Dundee’s School of Medicine, said unnecessary bed moves had adverse consequences for both patients and hospitals.
They said the reduction in bed numbers and rise in admissions had led to the practice becoming more common, especially for older patients.
This was despite the fact that such patients faced increased risks from being moved, such as changes to the environment increasing the danger of them suffering falls and delirium, both of which were linked to older patients suffering serious injury and higher rates of death.
The experts said “boarding” patients also moved them away from dedicated elderly care units, where they would receive a Comprehensive Geriatric Assessment (CGA). This method of care has been shown to reduce further hospital admissions and the need for institutional care.
They said evidence showed that when frail, older patients were looked after in a specialist unit they were 25 per cent more likely to survive and return to live an independent life.
Writing in the British Geriatrics Society’s journal Age and Ageing, Prof McMurdo said: “Boarding is sometimes viewed as a necessary evil – at least compared to the alternative of having no bed in which to admit patients from the overflowing acute admissions unit.
“Yet at a systems level, boarding appears to be a false economy – every ward move increases length of stay, thus exacerbating the very problem that boarding attempts to circumvent.
Advertisement
Hide AdAdvertisement
Hide Ad“Worse still, frequent moves around a hospital are likely increase the risk of infection transmission, a factor trusts have been advised to incorporate into bed management policies.”
Figures show a fall in hospital bed numbers in Scotland.
In the year ending March 2003, there were an average of 17,903 staffed beds in Scottish hospitals. But by March last year this had dropped to 16,503. At the end of March 2013, average bed numbers stood at 16,436.
At the same time, many health boards in Scotland have reported high occupancy levels, particularly during winter, which have led to wards having to find extra beds for patients.
Dr Witham said:”A recent survey of medical staff found that 92 per cent of doctors would refuse to have a relative of theirs boarded out – this hardly inspires confidence in the quality of care received by patients who are moved around.
“The majority of patients being boarded are frail, elderly and cognitively impaired, because most patients admitted acutely to hospital have these characteristics, and are likely to stay in hospital long enough to fall victim to boarding.”
Dr Witham said in the wake of the Francis report into unnecessary deaths at Mid Staffordshire NHS Trust, doctors needed to be “honest and open with patients and their families and explain the risks associated with unnecessary ward moves”.
Dr Neil Dewhurst, president of the Royal College of Physicians of Edinburgh, supported calls to reduce unnecessary ward moves for elderly patients.
“Such patients are likely to be the least likely to be able to cope with repeated ward moves,” he said. “Currently we have an insufficiency of properly supported acute beds to ensure these patients are treated in the right wards, by the right medical staff and at the right time.”
Advertisement
Hide AdAdvertisement
Hide AdMichelle Mitchell, of the charity Age UK, said older people often had the most complex care needs. “So it’s very disturbing to hear that they are regularly being moved to make space for new patients,” she said.
Scottish Labour’s health spokesman Neil Findlay added: “If measures are not taken soon, the issue of boarding is a crisis that will happen as we cope with an ageing population.”
Health Secretary Alex Neil said: “Scotland is the first country in the UK to deal with the issue of boarding.
“This work has already begun and is proving productive. However, there is more to be done, and this will involve reviewing the number and type of beds for acute care, ensuring there are enough consultants and nurses and having daily reviews of patients by consultants.”
SEE ALSO