Why medical staff in China spurned offers of psychological help over Covid – Dr John J Marshall
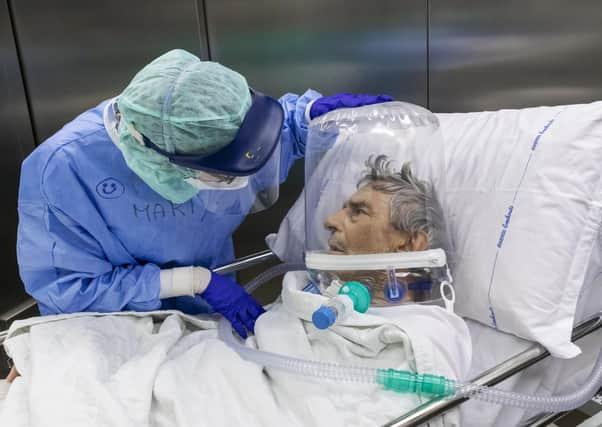

Some psychologists have been an unintentionally hidden menace in the unfolding Covid-19 crisis but they can be a force for good in the end.
Psychology came to the fore for the wrong reasons in this Covid-19 tragedy. Early on when the US government was forming its strategy, a social psychologist spoke about people being preoccupied with fears yet having a low probability of getting the disease – minimising the situation just when planning to mitigate the tsunami was underway. The UK was forming a ‘herd immunity’ strategy, informed by psychological nudge theory.
Advertisement
Hide AdAdvertisement
Hide AdTypically, nudge theory concerns itself with how governments can construct letters to taxpayers in a way that leads to increased tax returns or how to nudge people into washing their hands. With nudge ideas drifting into epidemiological territory, ‘herd immunity’ was born along with trying to “cocoon” the vulnerable against exponential virus spread. Instead, we could have been learning from what works among different nations. Dr Stuart Ritchie, a psychologist at King’s College London, has written about the dangers of trusting psychologists when it comes to virus epidemiology.
Psychologists are offering to help support those at the ‘frontline’, such as staff in intensive care units (ICUs). There is a tendency to think trauma is inventible in a disaster. The urge to counsel or support NHS colleagues making life and death decisions, communicating with families about their dying loved ones, or coping with the loss of patients they have ‘fought’ – it’s hard to avoid combat allusions – to save, is understandable.
Our intuitions are leading to helplines springing up, frontline distress services, well-being self-help packs, even ‘wobble’ rooms for staff needing emotional support with mindfulness colouring-in books – probably the last thing you would want to do. But our intuitions about this kind of help are plain wrong. Research from disasters and crises more often highlight resilience and mental health endurance. Some studies even describe post-traumatic growth, a positive psychological transformation following a massive life event. There are also risks to immediate debriefing professionals after a crisis which can worsen the emotional plight of health workers. There is nothing like your own family or networks to debrief to, if you want.
The vast majority can cope
In Wuhan, the source of the Covid-19 outbreak, psychological support systems were implemented. These included building a psychological intervention team, online courses for medical staff to deal with psychological problems, and a psychological hotline team, which provided guidance to solve psychological problems and stress management.
But medical and nursing staff did not use these services. When surveyed as to why they avoided them, people said they simply needed breaks that were uninterrupted, refreshments, enough equipment to keep them safe and the ability to communicate with families to reassure them. Their needs were more fundamental than psychological support.
Psychologists need to learn from the Wuhan experience because in a rush to support we can send the wrong message which could be heard as “you will need all these supports because we don’t think you can cope” when the vast majority do. Who’d want to be a ‘wobbler’ in the ‘wobble room’?
Where psychology can be of help is to challenge some of the language in health organisations as well as how we frame people’s experiences of Covid-19. The problem with the info blizzard on Covid-19 is how much of it is predicated on weasel words. The economist Fritz Machup defined weasel words as devoid of thought and sucking out content, like the obligatory war metaphors.
Dehumanising policies
With Covid-19, militaristic metaphors help us manage uncertainty. NHS staff are mobilising or deployed, just before the battle commences. They are at the frontline. Nurses are the unsung heroes marching to fight this disease. Presidents and Prime ministers declare war against a microscopic parasite invading our cells.
Advertisement
Hide AdAdvertisement
Hide AdThe problem with military metaphors is they can lead to dehumanising policies. Military language implies top-down command, to some degree necessary in a crisis but not the point of stifling individual creative solutions or action. NHS staff need to be trusted to make the best decisions they can. T–aking away autonomy in a high-stress emergency is one way to ramp up the risk of emotional problems down the line for our brave staff.
Professional key workers are at risk of moral injury where they are asked to work in ways that transgress moral, ethical or professional competencies. Moral damage leads to negative preoccupation and thinking. Moral injuries can occur if staff with little experience are asked to work in a high-stress, traumatic setting with no preparation or having to work without proper equipment. A recent article in the Lancet Journal describes a concerning example of moral injury in not being able to tell relatives that ‘we did all we could’ because resources are stretched beyond breaking point.
Social Darwinism
When someone like our Prime Minister suffers from the effects of Covid-19, he is a “fighter”. This could be heard by those with family members who tragically perished from Covid-19 as suggesting they gave up the fight. While the idea of a will to live might be match notions of fighting, the reality is that factors such as dosage of virus exposed to and underlying health problems are far more likely to affect what happens to someone with Covid-19.
The level of fight people have – whatever that means – is not a feature that stands out in Covid-19 survival statistics. This type of ‘individualist fighter versus implied failure’ mentality smacks of underlying ideas of social Darwinism, of the strong versus the weak. Yet we have seen how this virus causes misery for families of healthy victims.
Covid-19 is arousing our bodies fight-flight responses; the battle metaphors are no coincidence. People with HIV or cancer can experience unnecessary stress when pitted against battles to win or lose. Instead, we can learn from ancient Chinese medicine and their nuanced interpretations of war in terms of balance, harmony and a journey.
The challenge for all of us in these extraordinary times is managing deep uncertainty. When it comes to Covid-19, Plato’s phrase from more than 2,000 years ago, “The cure of many diseases is unknown to physicians”, is stark juxtaposed against our high-tech medical services.
Professionals and families are having the most daunting conversations about patients or family who are dying and, until there is an inquiry into the whole governmental strategy and its outcome, all that can be done is for everyone to bring as much humanity and compassion to these terrible times.
Dr John J Marshall is a consultant clinical and forensic psychologist
Comments
Want to join the conversation? Please or to comment on this article.
