Susan Dalgety: A country of 18 million – and just 39 dentists to treat them

Homba picked her head up from her chest, and with as much power as she could force out of her weakened lungs, she whispered hoarsely, “I’m a chief.”
Then she wiped her mouth as daintily as she could with hands almost paralysed by a series of strokes and dropped her head back on to her chest. “Tired,” she said, almost inaudibly.
Advertisement
Hide AdAdvertisement
Hide AdHomba will be 92 on her birthday, on July 4th, two days before Malawi celebrates its 55th year of independence from Britain. She is not Malawian, but was born in South Africa’s Eastern Cape and, as she used to proudly tell me, went to the same school as Mandela, “but he had left by the time I went there.”
She came to Malawi in 1954, with her long dead Malawian husband Roland, to help fight for her adopted country’s independence. Now she waits to die. “I am too tired,” she said.
She is one of a growing number of Malawians who suffer from hypertension and strokes. In the last 20 years, the number of people suffering a stroke caused by a bleed to the brain has gone up by a third. It is one of the biggest killers in Malawi, and a significant cause of disability.
High blood pressure is a growing epidemic, fuelled, like type 2 diabetes, another disease on the rise, by poor diet and lack of exercise, but also genetics. Africans, it seems, are more susceptible to hypertension.
Homba is lucky. She is the matriarch of a family that at the last count included ten grandchildren and 18 great-grandchildren. Her grand-daughters take turn to bathe her and massage her almost lifeless limbs. They tempt her appetite with beef and rice, spiced with chilli, and there is always someone there when night terrors wake her at three in the morning. “I think I am trapped in my coffin and can’t get out,” she told me once.
But for many Malawians, particularly the villagers who make up the bulk of the country’s population, a stroke is a life-destroying, if not life-ending, event. There are no disability payments from the Malawi government, no state pension, and the country’s first stroke unit is still a work in progress.
A group of British stroke experts from London and Liverpool have joined forces with Malawi medics to raise enough money to open the country’s first dedicated stroke unit, but they are still 8,176 bricks short. Meanwhile, an increasing number of people are struck down every day.
“Soon we will be able to research the causes of stroke and other inflammatory diseases such as cardiac disease and arthritis, thanks to support from Scotland,” says Dr Mwapata Mipando, principal of Malawi’s highly rated College of Medicine, as he showed me round the site for a new research lab.
Advertisement
Hide AdAdvertisement
Hide AdSo far so predictable. Rich country helps poor country with aid for basic health care. But this new partnership between the University of Glasgow and the College of Medicine, funded by the Scottish Government and the World Bank, is a world first.
The Blantyre-Blantyre project, as it has been dubbed, will directly benefit both countries. Its findings will help improve healthcare in Malawi, at the same time informing research into the, as yet unexplained, causes of poor health and low life expectancy in Glasgow and the surrounding area. This so-called ‘Glasgow effect’ sees a quarter of men die before their 65th birthday.
As Alex, the administrator for Glasgow University’s Wellcome Centre for Integrative Parasitology, showed me the site for the new state of the art microscope she had carefully packed for its flight to Malawi, I thought of David Livingstone – 160 years after the young medic from Blantyre set foot in Malawi, the two countries are collaborating on medical research that could saves countless lives in both countries. I think he would have approved.
He would most definitely have given Professor Jeremy Bagg the thumbs up. The cheerful dentist is on a mission to improve the oral health of Malawi children and train a new generation of Malawi dentists.
The Maldent project, also funded by the Scottish Government, is nothing sort of an oral revolution.
Over a (sugar-free) coke, Professor Bagg, who is head of Glasgow University’s Dental School, told me about the team’s plans.
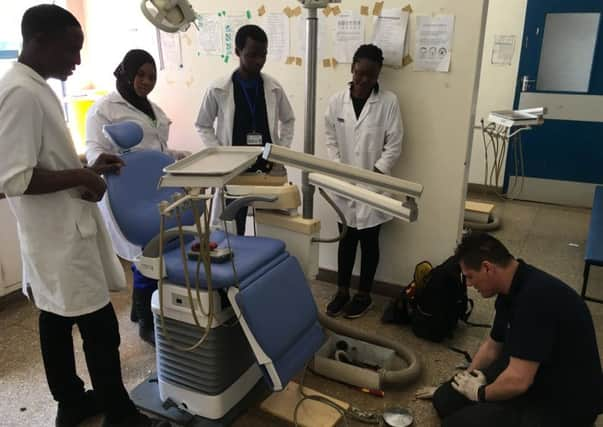
“There are 39 dentists in this country, for a population of nearly 18 million.” He paused while we both pondered the ridiculousness of that statistic. “And they were all taught outside of Malawi, in the UK or Australia.”
But no more, because from August this year up to 15 Malawians will embark on the country’s first dentistry degree at the College of Medicine, thanks to the Maldent project.
Advertisement
Hide AdAdvertisement
Hide AdSix schools in Northern Malawi will take part in a study of child oral health which will form the basis of a national campaign, inspired by the successful Childsmile programme. This has seen a significant decrease in tooth decay among Scottish children and saved Scotland’s health service up to £5 million a year since it was conceived in 2006.
“Don’t forget, untreated toothache can also kill,” grimaced Professor Bagg. “If an abscess travels down into your neck…” and he stopped, leaving the rest to my over-vivid imagination.
I have met some remarkable people this week, not least Professor Bagg. He could be enjoying his well-earned retirement, indulging in his love of cars. Instead, he is worrying how he can raise enough money to build a state-of-the-art dental school.
In her spare time, Alex, and her colleague Carole, raise money through their small charity Handbags for Malawi, which provides, amongst other things, a soft toy for a Malawi child to hug when they emerge from a malarial coma.
I listened in awe while Godknows Maseko told me about his family of 73 children, who he and his wife Helen have rescued from the streets of Blantyre – but more of their remarkable story later.
Everyone I met this week was full of love. Not a sickly, white saviour, post-colonial, patronising, fake love – but a genuine empathy for their fellow human beings.
As the liars and the braggers, the populists and the xenophobes, rage against our common humanity, trying to divide us for their own selfish ends, this week has restored my faith in people. And dentists.