John MacDonald: World’s health must become priority
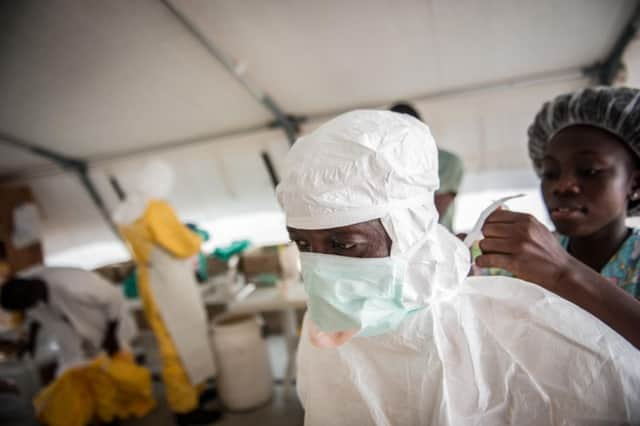

Tardily, the international response to the latest Ebola outbreak is gathering pace. The US has committed $1 billion (£621bn) in aid and will deploy up to 4,000 troops to affected countries, if required. The UK contribution will see the RFA Argus moored off the Sierra Leone coast, providing logistical support for hospitals and treatment centres to be built. By November’s end, around 750 British troops will be in Sierra Leone helping to tackle the outbreak, making it the UK military’s biggest current overseas deployment.
We can only hope that these measures are timely. Sierra Leone, having enjoyed a period of stability and economic growth after years of war, once more finds itself vulnerable. In Liberia, the worst-affected country, the public health system is disintegrating. Health workers are leaving their jobs, hospitals are closing. Across the affected region, people are staying indoors and not going to work. Children are being kept from school. The under-reporting of Ebola cases is thought to be rife. As societal deterioration unfolds, the UN World Food Programme is now concerned that chronic food shortages may hit West Africa.
Advertisement
Hide AdAdvertisement
Hide AdThe current crisis can be linked to a familiar villain – negligence on the part of richer nations. The Sars scare in 2003 spurred a revision of the International Health Regulations aimed at improving global disease surveillance and response. Crucial to this process was the richer nations supporting and working with the poorer ones. This clearly hasn’t happened as required. The nations currently affected by Ebola don’t have effective disease surveillance systems in place, nor do they have adequate medical and laboratory facilities. What we are witnessing now is the consequence of having an international disease monitoring and response system which prohibits the key at-risk nations from working effectively within that system. It represents, critics say, a clear failure of commitment by those nations best placed to commit.
As the focus now shifts to monitoring and prevention in 15 other African countries, some commentators remain sceptical about exaggerating the seriousness of the outbreak. The UN, on the other hand, warned this week the world has just 60 days to get Ebola under control, or face an “unprecedented situation for which we don’t have a plan”. Faced with having to choose between sceptical minimal engagement, and meaningful action, adopting the former position seems a fool’s choice.
What is required now is not just a Herculean effort to de-escalate the current crisis but also a clear acknowledgement of why things stand as they do.
Whilst we should be wary of over-simplifying, a significant part of the solution is fairly straightforward. The World Health Organisation (WHO) needs to see an end to the budget cuts which have slowly enfeebled it over decades. Short term, it needs sufficient funds to get more trained people on the ground in Central and West Africa, and to keep them there. Longer term, it needs to be sufficiently financed so that it can maintain an effective global disease surveillance and response programme.
If that sounds fairly straightforward, the difficulty may lie in convincing those who have underfunded the WHO in recent times – its 194 member states. Any bolstering of the WHO will require a sea change in how its work is regarded. In short, the world’s leading nations will have to start taking lethal communicable diseases as seriously as they do security threats, such as international terrorism.
When we look at the impact of the current outbreak, we can see that there is much to justify this necessary change in perspective. Notwithstanding the health risks attached to the accelerating transmission of the virus, the prospect of state failure in West Africa is pronounced. We have become all too familiar with the effects of such failures in recent years. They create wars and refugees, decimate the physical environment and provide opportunities for extremism to flourish. These events invariably impact heavily on neighbouring states and entire regions. Ultimately, the ripple effects are rarely confined to the African continent.
The US and the UK would be crucial participants in any serious commitment to re-bolster the WHO and its work. Both countries already demonstrate a willingness to commit vast sums of money to address notional threats on other continents. Even at the height of austerity, funding continues to flow towards “anti-terrorism” endeavours across the Middle East and Africa. At this point, it is difficult to argue that addressing infectious diseases should not receive a similar commitment. To renege on addressing this issue will simply put problems on hold. The current outbreak, or even the next one, may not turn out to be the stuff of disaster movies but if the international community won’t commit to the implementation of an effective global monitoring and response system, we will continue to be dragged back to where we are now: watching innocent people die, affected nations fragment, worrying about whether the disease will reach us, and spending money recklessly in the desperate attempt to play catch-up.
The World Bank estimates that 90 per cent of the costs of any outbreak “come from irrational and disorganised efforts to avoid infection.” If the moral imperative to commit to this issue is not in itself sufficiently moving, then the economic and security imperatives surely dictate the wisest path to follow.
• Dr John MacDonald is Director of the Scottish Global Forum, www.scottishglobalforum.net @1johnmacdonald