Innovative and imaginative policies are required to relieve the burden placed on GPs - Andy Drane
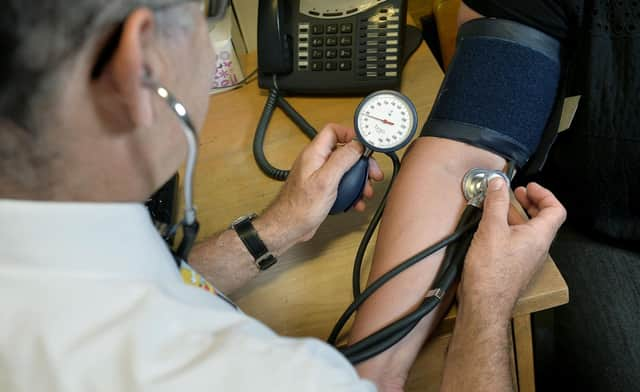

A poll published near the end of 2020 in GPonline revealed that 81 per cent of GPs had seen their workload rise since the pandemic hit, with a third describing work-related pressure as 'very high'. The situation is unlikely to improve with the UK managing a second wave of the virus.
GPs throughout the UK have been operating in a difficult environment long before Covid-19 ever entered our lexicon. While the added pressure brought on by the pandemic has triggered an immediate crisis for those within the profession, none of the legacy issues have gone away either, presenting a wider threat to public health and wellbeing.
Advertisement
Hide AdAdvertisement
Hide AdAs GPs continue to get older, there aren’t enough newly-qualified candidates emerging as replacements, nor will there be for some years to come. Training more doctors takes years: those who start a medicine degree this year will not reach fully fledged partner level until after 2030 at the earliest.


The option of recruiting experienced doctors from abroad is a typically costly process which also denies poorer nations of much-needed medical skills.
While some UK doctors have postponed retirement to help during the pandemic, for others it’s hastened their plans to step down from the profession. With the second wave of Covid placing even greater burdens on the profession, I would anticipate that once they get the chance to draw breath, significant numbers of GPs will decide it’s time to move on.
Here in Scotland, the challenging task of GP recruitment has been further complicated by the Scottish Government’s attempted integration of health and social care alongside the implementation of its new GP contract. Under the new agreement, GP practices will continue to operate as private businesses with the partners’ remuneration dependent on their level of profitability. Policy underpinning the new agreement is supposed to offer further Government support by removing elements of the risk of running a business from GP practice partners, allowing them to focus more clearly on meeting patient needs.
As well as making more funding available, the new GP contract also reinstates the principle that doctors are expert medical generalists supported by a raft of healthcare professionals and should therefore only focus on those patients who actually need to be seen by them. At least that’s the theory.
Despite the pandemic’s impact on the entire health service, there have been recent signs that some Health Boards are attempting to implement these policies although the pattern across the country is patchy and progress is, perhaps understandably in the current climate, proving slow.
However, if Scotland is to avoid post-Covid GP shortages, further actions will be essential. Creating a vibrant and stable working environment for GPs and other healthcare professionals is a critical part of addressing improving the country’s underlying health issues. Along with ensuring that all Health Boards take a consistent approach in implementing the new contract, the Scottish Government must also deliver on its key support policies.
Meanwhile, the Conservative Government at Westminster needs to focus on UK-wide issues which prevent older, experienced GPs from working. The Chancellor’s March 2020 budget took some steps towards addressing aspects of the pension crisis where currently doctors’ earnings are super-annuable at fixed percentages. Covid has diverted debate from these steps but issues still remain, particularly around lifetime allowance limits.
Advertisement
Hide AdAdvertisement
Hide AdIncentivising medical students into a career within general practice is also needed along with rules requiring UK-trained doctors to remain working here for a minimum period after qualifying.
The post-Covid world represents real opportunities for the Government and the profession to reimagine how services are delivered. Challenging as the pandemic has been there has been new learning for everyone, the health sector included.
The strain on GPs is likely to continue beyond Covid if policymakers fail to deploy innovative and imaginative policies that reduce the increasing burden they’re facing. Given the essential frontline role of GPs in promoting public health, it is a challenge which must be met with vigour and urgency.
Andy Drane, partner and GP practice adviser, Davidson Chalmers Stewart