Dani Garavelli: Scotland’s drugs tragedy demands hard questions not glib answers
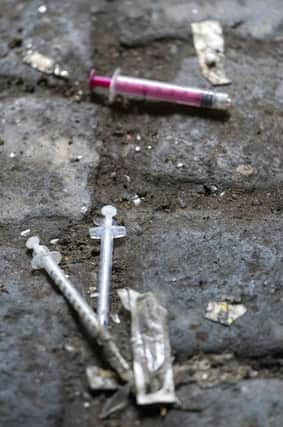

The statistics were no less shocking for being widely anticipated. Last year, 1,187 people in Scotland died drugs-related deaths. It was the highest toll since records began in 1996 and earned us the No 1 spot on a European league table no-one wants to top.
More people died from drugs last year than suicide, but what is this reckless consumption if not an expression of hopelessness; a sort of suicide by increment?
Advertisement
Hide AdAdvertisement
Hide AdThese users are not just numbers; they are individuals,who have been robbed of their futures, and they leave behind families devastated by their passing. Many of them have histories of trauma and homelessness and the failure to prevent their deaths is a national scandal of such significance it behoves everyone involved to set aside their political allegiances for the common good.
Instead – sadly, yet predictably – many saw the grim news not as a catalyst for sober reflection, but as an opportunity to grind their axes in the never-ending constitutional debate.
Nationalists put the blame squarely at the door of the UK government which has blocked proposals for a drug consumption room – a centre where drugs can be injected under the supervision of trained staff – in Glasgow. These figures were, they opined, further proof of the need for Scotland to cut itself free from the rest of the UK and take control of its own drugs policy.
Unionists, meanwhile, savaged the Scottish government, which has cut funding for rehabilitation services by 6 per cent since 2015, and pointed out that Scotland’s death rate is three times that of England’s, despite being bound by the same legal framework.
On the fringes, this buck-passing produced the usual foaming-at-the mouth delusions. Gaining some traction in some quarters was the claim that the Scottish figures were only higher because they were differently collated. At the other end of the spectrum, efforts were made to conflate the rise with the Scottish Government’s minimum pricing on alcohol policy (a suggestion immediately dismissed by health policy analyst Andrew McAuley).
But the blame game wasn’t confined to extremists. The SNP’s own Twitter account focused heavily on Westminster’s recalcitrance, while Tory MSP Murdo Fraser bemoaned the “moral bankruptcy” of the SNP for using the deaths to score a “constitutional point”, while, er, trying to score a constitutional point.
The problem with this binary response – other than its cynicism – is that it militates against any thoughtful analysis of an incredibly complex situation. Why is Scotland’s drug deaths rate worse than other countries’? The answer is multi-layered. It has proportionately more areas of intense deprivation than England and a high number of men in their 30s and 40s whose long-term use of heroin has left them with multiple health problems. But in recent years it has also seen a rise in poly-drug use – largely benzodiazepines on top of heroin/methadone – making it harder to implement effective harm reduction policies.
It is true, as the SNP contends, that the countries that have had the biggest success in tackling fatal overdoses have done so by de-stigmatising drug use and shifting from a criminal justice to a public health approach.
Advertisement
Hide AdAdvertisement
Hide AdIn Portugal, where the use of heroin spiralled in the 1980s, a handful of pioneers set up needle exchanges and methadone treatment programmes. In 2001, the decision was taken to decriminalise the possession and consumption of all illicit substances, so users were no longer scared of seeking help. Drugs-related crime and deaths, HIV and hepatitis C infections and the prison population have all dropped dramatically as a result. Today, there are needle exchanges and drop-in centres and outreach workers who take state-issued drug kits to open-air injecting sites.
Westminster’s resistance to this more tolerant public health approach is frustrating; but there are also issues the Scottish Government could address within the existing legislation.
The Scottish Drugs Forum, for example, says those on the methadone programmes in Scotland are often receiving suboptimal doses (so topping up with other substances) while newly referred users are waiting up to six months to access treatment.
According to McAuley, there is also a problem with treatment retention rates, with a need for more outreach work and the removal of sanctions for missed appointments..
“The system is fragmented, under-resourced and is the same as it was 20 years ago, but people are using much more lethal poly-drug combinations now,” he said. “They need the wrap-around services because the cases are much more complex. But these are the things that get stripped out when funding becomes tight.”
The Scottish Government has already demonstrated how radical initiatives can be introduced with its existing powers. In 2010, it set up a national programme to dispense Naloxone – the antidote to an opioid overdose – in prisons and beyond; in five years, more than 34,000 kits were handed out, leading to a drop in drugs-related deaths amongst those who had recently left jail (a cohort which is particularly susceptible).
Plans for a Heroin Assisted Treatment (HAT) facility in the East End of Glasgow are also well-advanced. HAT facilities differ from drug consumption rooms in that the opiate being injected on-site is legally prescribed diamorphine, as opposed to illegally purchased street heroin; as a result no legal exemption from Westminster is required.
HAT facilities, however, are intended for use only where methadone programmes have failed and have limited capacity, so investment in third sector initiatives, such as café-style clinics, is also critical.
Advertisement
Hide AdAdvertisement
Hide AdDrug Consumption Rooms have proved their worth in Germany and Luxembourg. But there are no such facilities in Portugal where success is attributed to a less judgemental attitude towards drug users and the tailoring of treatment to individual needs.
Some experts believe the constitutional tug-of-war around the proposed Glasgow centre is inflating its potential significance and deflecting from a more holistic approach that recognises the connection between drugs use and other social factors such as poverty and unemployment.
Last week’s drug deaths figures should have shaken the Scottish political establishment to its core, yet the response was lacklustre. If this is truly being treated as a national emergency, why weren’t Nicola Sturgeon, Jeane Freeman and Humza Yousaf taking the lead? Why was it left to Joe Fitzpatrick, minister for public health, sport and wellbeing, to respond?
I would also question the need for the new task force to gather and publish good international practice when it is already so well-established. A more productive line of attack might be to address the way methadone treatment continues to carry a stigma in Scotland it long ago shed in other countries. This stigma – the notion that drug users are being “parked” on methadone as opposed to viewing it as a legitimate and effective form of treatment – contributes to suboptimal prescribing as GPs feel a pressure to demonstrate their patients are “making progress”.
More than anything else, however, what is required is for politicians and activists to stop weaponising the deaths of some of our most vulnerable citizens; to resist the temptation to turn this into another constitutional bun fight, and to approach Scotland’s complex poly-drugs problem with open minds, good will and a commitment to collaboration.