Covid Inquiry must focus on what China got right and UK got wrong during pandemic, not who's to blame – Professor Anthony Seaton
As we watch the Covid-19 Inquiry unfold, it is well to remember that it was never going to be easy. It was to prove the UK’s greatest challenge since 1939.
The 1918/19 influenza was the last pandemic that killed millions, including my grandmother. For decades, I taught medical students about our interactions with microbes, part of Darwinian competition for nature’s resources. This is an unequal struggle, bacteria and viruses mutating rapidly whilst we rely on ingenuity in detecting illness early, tracing contacts, and finding cures and vaccines. But this will never be enough; pandemics still occur and modern travel has increased the risks.
Advertisement
Hide AdAdvertisement
Hide AdIn December 2019, we heard of the new epidemic in China. Could Covid be as awful as 1918/19? We had no vaccine against this new virus. In January, I read the reports from China with increasing anxiety. They quickly identified the viral genome, enabling work on designing a vaccine, but they detected something very worrying.
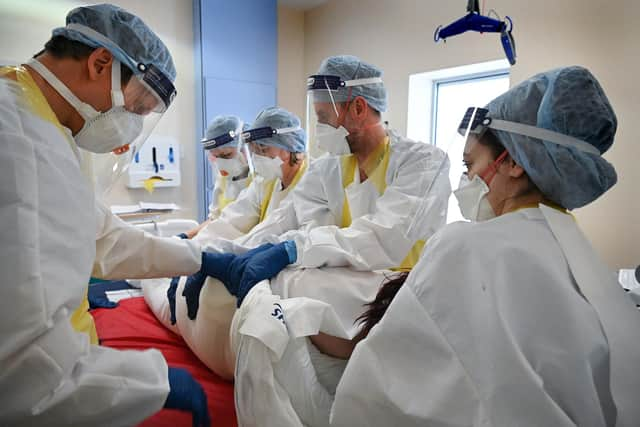

The infection spread rapidly and could pass to others before symptoms developed, something to fear in a new virus. Epidemic control depends on early detection of infected people, their isolation, and tracing contacts. If symptom-free people can pass the infection on, it decreases our ability to prevent mass infection.
Very hard to control
The new virus was a relative of the common cold that had been extensively studied and was transmitted on breath. Papers from the Far East showed that it was highly infective, with a 15 per cent fatality rate in old people but little serious illness in children. It was clearly going to be very hard to control.
These were the basic facts available to those responsible in February 2020. We still had time to prepare for it and I was reasonably optimistic that we would do so. I was wrong. Over January and February, the virus spread through the world, aided by travel associated with Chinese New Year. China and then Taiwan controlled it with the early deployment of classical public health responses, a very compliant population and th euse of sophisticated IT, keeping their infection rates and mortality under control. But the full horror of the infection in a country with poor public health systems became apparent as it reached Italy, where the health services were overwhelmed.
From early March 2020, I tracked the course of this modern plague across the world and wrote a series of articles, based on my understanding of particle transmission, to explain the precautions necessary to minimise personal risk, having noted the lack of adequate advice from governments at that stage. By mid-March, the Prime Minister seemed to wake up to the reality of the situation but was unconvincing on television and plainly needed to be accompanied by experts.
Fortunately, plenty were available to him, though initially in a secretive committee called Sage. At that time, the Scottish Government appeared not to have any experts on epidemics, virology or personal protection in its service and the public health response seemed lacking.
My advice at the time
From early March, the advice I took myself and gave my readers can be summarised simply. You catch this disease by inhaling other people’s exhaled breath, and the longer and closer your exposure, the greater the risk. The risk is much greater indoors, in crowds and in poorly ventilated buildings, so avoid such situations, especially if you are over 65. And if you start to feel ill, isolate yourself from other people until you feel better. I did not use my ticket at Murrayfield that week.
By then, it seemed obvious that the NHS was going to be overwhelmed by a failure of public health. Senior medical and nursing staff spontaneously took control, expanding intensive care capacity, shifting their jobs from routine work and going where they were needed. Most unfortunately, the protective equipment provided for staff, notably face masks, was useless save that used in intensive care, and this was reflected in the awful rates of infection among doctors and nurses on the wards and in social care.
Advertisement
Hide AdAdvertisement
Hide AdThis was an avoidable disaster based on a misunderstanding of the mode of transmission, and was exacerbated by poor infection control among hospital staff. Later, that persistent misunderstanding of transmission led to the UK Government’s disastrous “eat out to help out” initiative.
Altruism of NHS staff
Concerned about the economy and under pressure from big businesses such as ”hospitality”, politicians hesitated in locking the UK down when infections were increasing exponentially. Matters were made worse by years of reduction of NHS bed capacity and of local public health functions, by the transfer of infective patients from hospital to the overwhelmed and largely under-protected care sector, and by initial unavailability of a fast, reliable test for the virus. All were derived from efficiency decisions by previous governments. Where the Chinese succeeded, we failed.
Many lost close relatives during the pandemic, but we survived and must be grateful for positive achievements. First, the altruistic way that NHS staff coped with the onslaught in the first wave. Second, the international effort, combining advances in genetic engineering and nanotechnology, that produced effective vaccines within a year. Third, the combination of epidemiological and NHS expertise in clinical trials to test the vaccines, discover effective treatments and rule out ineffective ones, Fourth, despite attempts to engage for-profit organisations in case-finding and vaccine administration, the brilliant role of the NHS in vaccinating us. And finally, the many poorly paid people in essential jobs, who delivered the services that we relied on and often caught Covid as a consequence.
It is now for the inquiry to work out the longer-term lessons on pandemic management and not to be diverted by a hunt for whom to blame. They need to study how the Chinese got it right. When the next one comes, we must be better prepared.
Anthony Seaton is a retired chest physician and professor of environmental medicine
Comments
Want to join the conversation? Please or to comment on this article.