Covid: Bill Gates' internationalism, not Donald Trump's nationalism, is vital for fight against the pandemic – Susan Dalgety
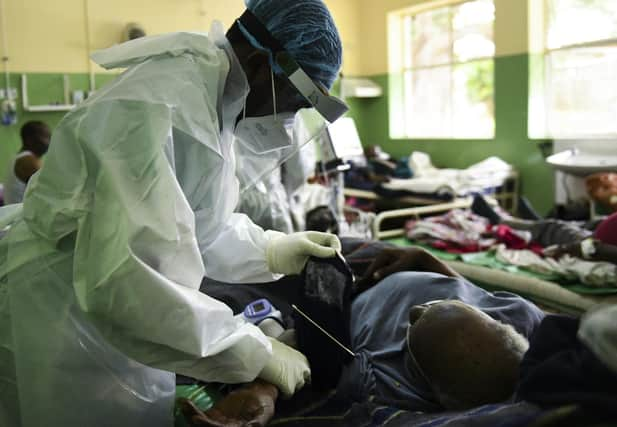

There are no high-tech ventilators, specialist intensive care beds, or staff trained in the latest coronavirus treatments. Just eight beds, a team of dedicated but exhausted medics and around 15 cylinders of oxygen.
By the time a patient ends up in the isolation unit, they are very ill, barely able to breathe. Oxygen offers their only chance of survival. But according to Tom Hunt of Medic Malawi, a British charity working in the area, each patient can use three cylinders of oxygen in 24 hours.
Advertisement
Hide AdAdvertisement
Hide Ad“That means 24 cylinders are needed every 24 hours,” he explains by WhatsApp. “We have 15. The nearest place we can refill the cylinders is Lilongwe, a two-and half-hour drive away. A refill costs £70, a new cylinder is £280 if you can find them.”
Four nights ago, Tom and the local MP Madalitso Kazombo spent hours on their mobile phones desperately trying to track down spare oxygen cylinders as a dangerously ill patient’s supply was about to run out.
National emergency
“We finally managed to source new cylinders,” explains Tom. “And Madalitso drove them back from Lilongwe in the middle of the night. But the situation is desperate, we are working hand-to-mouth. Specialist care across the country is limited, and here in Kasungu, Covid patients often arrive at the district hospital too late, unable to breathe. Oxygen is their only hope.”


Tom and Madalitso have set up the Kasungu Oxygen Task Force to bring key people in the area together to find a solution to the immediate crisis, and also to work on a long-term solution. “Oxygen was in very short supply, even in non-Covid times,” says Tom, who has been living in Malawi with his wife and young family since last November.
Malawi’s first wave of coronavirus barely caused a ripple. During 2020 there were only around 5,000 cases, with fewer than 200 deaths. A young demographic, more than half the population is under 18, the outdoor lifestyle of most households, and possible T-cell immunity were just some of the reasons offered for the low numbers.
Malawian friends looked on aghast as the UK death toll mounted. “How can it be? You’re a rich country, why are so many people dying?” they asked. “It’s the white man’s disease,” said others.
Then a few weeks ago the numbers started to rise exponentially, driven by the South African strain. President Chakwera declared a national emergency on 12 December, closing schools, making masks mandatory and setting up field hospitals in the main cities.


"We presently find ourselves in one of the darkest hours in our nation’s history. We have entered the eye of this pandemic's storm,” he warned a fearful nation.
Incredible fundraising efforts
Advertisement
Hide AdAdvertisement
Hide AdThe crisis even prompted parliamentarians from Holyrood and Westminster to set their differences aside to host a meeting two weeks ago, where the Malawi health minister, Khumbize Kandodo Chiponda, Scotland’s international development minister, Jenny Gilruth, and 250 other people agreed to join forces to help Malawi get through their second wave.
The UK government, through global body Covax, has already promised 1.5 million doses of the Oxford Astra Zeneca vaccine, which should reach Malawi next month, but the immediate, desperate, need is for oxygen. Even where there are cylinders, there is often a shortage of basic supplies such as tubing, filters, facemasks and oximeters.
The Scotland Malawi Partnership is supporting efforts by Scottish organisations to help, with a focus on refurbishing the country’s existing oxygen concentrators. And a group of Malawians have got together to raise money for essential equipment. Covid Response has to date raised 170 million kwacha (£170,000), from private donations. One of the organisers, Dr Thandiwe Hara, says the response has been incredible.
“This is the first time Malawians have come together to raise funds like this,” she says. “The donations are way beyond what we had hoped for. We have money from big and small businesses. Children have made masks, sold them for 50p and donated a fiver.”
Trapped in our homes, staring out at the grey skies, counting down the weeks or months until we get the blue envelope with our vaccine appointment, it is all too easy to forget that we are not the centre of the universe.
Even if every person in Scotland is vaccinated by the end of the year, coronavirus will be remain a global, and therefore a local, problem for years to come.
International co-operation is vital
Borders are meaningless in the face of a deadly virus; witness the journey of the UK strain from Kent to Kentucky. Climate change doesn’t require a passport to wreak its havoc, and economies are dependent on each other for markets, supply chains, even labour.
If humanity is to survive, literally, then countries are going to have to co-operate better. The pandemic has shown what we can achieve. As Bill and Melinda Gates wrote in their annual newsletter, published a few days ago, no one country or company could have developed vaccines so quickly on its own.
Advertisement
Hide AdAdvertisement
Hide Ad“Funders around the world pooled resources, competitors shared research findings, and everyone involved had a head start thanks to many years of global investment in technologies that have helped unlock a new era in vaccine development,” they write.
The basic instinct of politicians is to put their own people first, but when patriotism morphs into nationalist populism, as it did in America under Trump and his “America First” doctrine, it becomes dangerous.
President Joe Biden’s first foreign policy speech promised the world’s biggest economy would “engage with the world once again, not to meet yesterday’s challenges, but today’s and tomorrow’s”.
It’s a welcome start, but it is incumbent on all of us, not just world leaders or billionaire philanthropists, to work together. In these new times, as Malawi’s Covid Response group says on its website, it's all hands on deck.
You can donate to the Medic Malawi oxygen appeal and the Covid Response group
A message from the Editor:
Thank you for reading this article. We're more reliant on your support than ever as the shift in consumer habits brought about by coronavirus impacts our advertisers.
If you haven't already, please consider supporting our trusted, fact-checked journalism by taking out a digital subscription.
Comments
Want to join the conversation? Please or to comment on this article.
