How Clyde shipyard technology created the ultrasound

TOM Brown vividly recalls his first encounter with the experiments in ultrasound being carried out in the Western Infirmary in Glasgow more than half a century ago. An engineer with Kelvin and Hughes, a company specialising in sonar and radar, he had heard doctors were using equipment designed to look for cracks in metal on human beings and more or less invited himself along for a look. But the bizarre contraption he saw when he was ushered in would have been more at home in a mad scientist’s lab than a working hospital. In the corner of the room was a clapped-out black-crackle-painted flaw detector, together with a precarious arrangement of glass cylinders, water jugs and jars of Vaseline.
The tests on the patient’s abdomen, carried out by the regius professor of midwifery Ian Donald, were nothing short of farcical. The procedure involved so much sloshing about of water that everyone got soaked and the echoes created as the sound waves bounced off the internal organs appeared on the screen as a series of virtually indecipherable spikes. Yet, inauspicious as it seemed, the demonstration was to mark the start of a fruitful partnership.
Advertisement
Hide AdAdvertisement
Hide AdThough others mocked, Donald and Brown were united in their belief that the techniques which allow bats to locate their prey and ships to avoid collisions could be adapted to scrutinise the internal workings of the human body. Cobbling together spare parts on a limited budget – and using chains and sprockets from a Meccano set – they built a contact scanner capable of distinguishing fibroids from ovarian cysts and tumours and eventually of monitoring the progress of the unborn child.


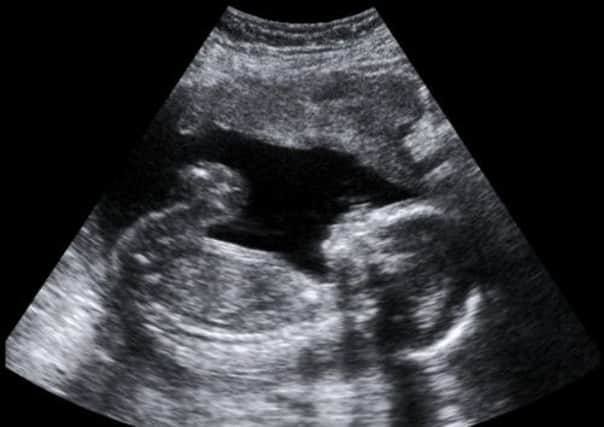
Fifty-six years later, life without ultrasound is unimaginable, especially in the field of obstetrics. For a pregnant woman the first scan, routinely carried out towards the end of the first trimester, is a ceremony as potent as anything the ancient Egyptians with their herbs and incantations had to offer; and like all symbolic events, it comes with its own rituals: the consuming of water (which improves the picture); the intake of breath as cold gel hits bare flesh; the pummelling sensation as the probe is passed across the stomach; and then – if all goes well – shadows on a screen, which materialise into recognisable shapes, a head, limbs, a sucked thumb.
The image of the unborn baby in the womb is both universal and intensely personal; quotidian and sacred. Routine though the procedure now is, the idea that, weeks before a woman first feels her baby move, she can see it wriggling about inside her is still nothing short of phenomenal.
Tomorrow, a book which explores the way ultrasound has revolutionised the care of pregnant women will be launched at Glasgow University. Imaging And Imagining The Fetus charts the journey from the first realisation that it could be used to locate the position of the baby’s head to now, when it is crucial for detecting foetal abnormalities or conditions, such as placenta previa, which place the mother or baby at risk. But its authors Malcolm Nicolson and John Fleming, the engineer who designed the first scanner to go into commercial production, also touch on the complicated legacy of a technology which been used as a pawn in both sides of the highly polarised abortion debate and exploited by cultures where boys are valued more highly than girls.
Ultrasound’s capacity to detect foetal abnormalities, combined with the 1967 Abortion Act, means parents can now choose to terminate pregnancies which will result in a severely disabled child. But pro-lifers have also used the images to present the foetus as an independent entity with its own human rights; in some American states, women seeking abortions are now obliged by law to view their own ultrasound scans before the procedure can be carried out.

Equally controversial is the issue of gender selection; underground clinics – which offer scans to determine the sex of the foetus and on-the-spot abortions for girls – are flourishing in India and China, with the result that both countries now suffer a demographic imbalance. “This is a major problem in the East,” says Nicolson, a professor of the history of medicine at Glasgow University. “In India, it is illegal to tell parents the sex of the foetus, but there are codes the scanning personnel use – if it’s a female foetus, they will tell the parents to expect serious expenditure; if it’s a male foetus they will hand them sweets, which is a sign of celebration.”
Donald, a devout Christian who died in 1987, would have been appalled. “But the history of ultrasound is full of unexpected twists and turns,” Nicolson says. “This is just one example which demonstrates the uses to which technology is put are not determined by its originators.”
Having worked on radar systems while serving with the RAF, Cornwall-born Donald arrived in Glasgow convinced high-frequency soundwaves could be used to aid medical diagnosis. The story of how he realised his dream is one of risk and innovation, full of maverick personalities, colourful anecdotes and conventions defied. There’s the oft-told tale of how Donald, inspired by seeing a worker at the industrial fabrication firm Babcock and Wilcox test a flaw detector by bouncing it off his thumb – packed his car boot full of freshly removed cysts and tumours and headed for the yard, where he conducted tests using a lump of steak as a control material. Or the one where, in need of a flexible membrane to hold water, he sent a visiting South African professor into a shop to buy condoms.
Advertisement
Hide AdAdvertisement
Hide AdIt wasn’t until Brown, who had already designed a mechanised flaw detector at Kevin and Hughes, joined the project, however, that it began to gain momentum. The only member of the original team still alive, the 80-year-old revels in telling how, days after the demonstration at the Western, he secured a newer, more sophisticated flaw detector from a former boss, loaded it into a taxi and then onto a patient cart and delivered it direct to Donald’s gynaecology clinic. Working days at the factory and evenings at the hospital, he helped adapt the machine for medical use. He built a Perspex tank to replicate the conditions inside the human body and procured an oscilloscope camera so they could record the echo traces on film. Gradually, the medics learned how to differentiate between different types of growths. A turning point came when they discovered a woman diagnosed with terminal stomach cancer actually had an ovarian cyst, which was then removed.
But while Donald – with colleague John MacVicar – were consumed with exploiting the potential of the existing equipment, Brown had something more cutting edge in mind. “I realised what was needed was some sort of pictorial display so you could see where the echoes were coming from,” he says. By the end of 1957, he had built a prototype B-mode scanner which could translate information on the echoes into a two-dimensional image. The following year the team’s paper – Investigation of Abdominal Masses by Pulsed Ultrasound – was published in the Lancet and the significance of the technology was accepted by the medical community.
Today ultrasounds are the second most common medical tests after X-rays, with more of them carried out each year than MRIs and Cat scans combined. According to the British Medical Ultrasound Society, the technology is used to detect testicular cancer, bladder conditions, thyroid problems and to locate the right spot for cortisone injections after neck and shoulder injuries. However, early on it became clear its principal use would be in the monitoring of pregnancies, and by the late 1970s it was already a key component of ante-natal care. Today every expectant woman in the country receives at least two scans, at 12 and 20 weeks.
In the beginning, everyone involved took enormous pride in their success. “I remember sitting on a bus and hearing two women talking about their scans and that’s when I began to realise what we had achieved,” says Brown. But, as society changed, Donald, a High Church Anglican, began to become disaffected. So vehemently did he oppose terminations, except in cases of severe disability, he took a petition protesting against David Steel’s bill round a labour ward. After it became law, he organised ultrasound screenings for women who planned to terminate their pregnancies.
“The net effect of the introduction of the ultrasound scanner was the rigorous imposition on the foetus of a reductionist discrimination between the normal and the pathological, which Donald found repugnant,” Nicolson says. In the late 1970s, he questioned whether – if he had his time again – he would choose to specialise in gynaecology and obstetrics. “My own personal fears are that my researches into early intrauterine life may be misused towards its more accurate destruction,” he wrote. “I myself would not like to feel I had contributed to a Huxleyian Brave New World.”
For many years Brown too was conflicted. As the technology flourished, he felt the doctors were being given all the credit while his contribution was ignored. His resentment was fuelled by the withdrawal of funding for a project to market his 3D scanner and by periods of unemployment interspersed with casual work in the oil and gas industry. But then, in 2007, a few years after he retired to Kinghorn in Fife, ultrasound gave him a personal legacy: at his pregnant daughter Rhona’s 20-week scan, a sharp-eyed sonographer spotted something unusual and she was diagnosed with vasa praevia, a rare condition which if undetected can lead to the baby bleeding to death immediately after delivery. As a result, she had a Caesarean section at 37 weeks and gave birth to a healthy son, named Tom after his pioneering grandfather.
Away from the central protagonists, debate over ultrasound continues to rage. Although its safety is rarely challenged, some oppose the increased medicalisation of pregnancy, while others say false positives (where the scan raises fears which later prove to be unfounded) leads to unnecessary worry which can continue to affect the woman after the birth. Nicolson dismisses critics who claim the growth of the ultrasound industry is being driven by commercial imperatives rather than the wellbeing of the patient, but even he is concerned by the number of private clinics which carry out 3D scans, not for clinical reasons but to provide the parents with hi-tech keepsakes. Despite these reservations, Nicolson believes ultrasound has changed the experience of pregnancy for the better. “Women report an emotional response to seeing the foetus on the screen, particularly a moving image,” he says. “Even if the news is bad, most say they would prefer to know it earlier rather than later, so they can prepare for the future or make difficult decisions.”
Towards the end of the book, the authors describe the experience of a couple who decided against abortion even though they were told their baby had no kidneys and would not survive. From that point on they came for regular scans which, their obstetrician said, allowed them to “pour 40 years of love into 20 weeks of pregnancy”.
Advertisement
Hide AdAdvertisement
Hide AdAs Nicolson points out, the ultrasound image is not a one-to-one representation of the foetus but “a signal received from particular interfaces with it”. To that extent it is an illusion. But it is a powerful illusion, with the capacity to arouse the most profound emotions in the beholder. Viewed like that, it is little wonder it has so captured the human imagination.
Twitter: @DaniGaravelli1
• Imaging And Imagining The Fetus is published by John Hopkins University Press