Patients experienced ‘lack of privacy and dignity’ in Forth Valley Hospital, report finds
On visits to Forth Valley Royal Hospital in April, Healthcare Improvement Scotland (HSE) inspectors found that most wards had increased the number of patient beds to meet the higher demand on the hospital.
At that time, the infirmary met the criteria for “black status”, the Scottish Government’s highest risk level, and NHS Forth Valley was experiencing increased patient numbers, additional delayed discharges and high levels of staff absence.
Advertisement
Hide AdAdvertisement
Hide AdMost four bedded bays at the hospital had been increased to accommodate five beds, meaning there could be up to five additional patients in each ward.
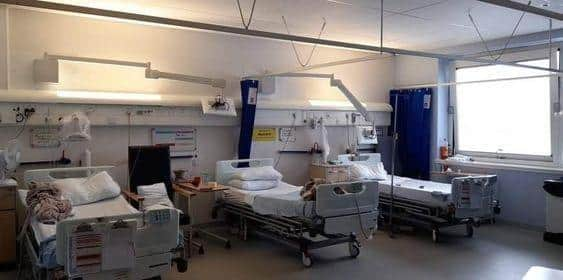

The HSE report said that patients in wards where extra beds had been introduced did not always have access to the same facilities such as televisions, call bells, space and curtain screens which “sometimes resulted in a lack of privacy and dignity”.
Inspectors also raised a serious concern around the use of treatment rooms as non-standard care areas for in-patients.
Donna Maclean, HSE head of service, said: “At the time of inspection, Forth Valley Royal Hospital, was experiencing a significant range of pressures associated with Covid-19, including increased hospital admissions, increased waiting times in emergency departments and reduced staff availability.
“During our inspection, we saw many good interactions between staff and patients, and observed examples of good team work and communication. There were also positive comments made by patients about the staff who provided their care.
”During our inspection, we escalated a number of serious concerns to NHS Forth Valley through our escalation process, some of these concerns included ward doors within the hospital being locked, without the process within the Board’s own locked door policy being followed.
“Another concern related to patients being placed in additional beds and non-standard care areas to accommodate increased patient numbers.
“The additional beds and non-standard care areas raised a number of concerns such as: lack of accessibility for cleaning, patient placement, access in an emergency, and patient privacy and patient dignity.
Advertisement
Hide AdAdvertisement
Hide Ad“Some staff we spoke with shared their concerns and feelings of being overwhelmed, particularly in relation to the additional beds and workload and they expressed feelings of frustration at staffing levels.”
Inspectors observed that some ward treatment rooms were being used as single rooms to accommodate patients overnight.
These rooms would normally be used for a short procedure or treatment for a patient attending the ward, however, they found one patient being cared for in a treatment room, a non-standard care area, for 12 days.
The report stated: “The patient told us they were unhappy with this. NHS Forth Valley’s policy states that the longest stay in the treatment rooms should be 24 hours.”
The unannounced inspection visit to the 687-bed hospital in Larbert, near Falkirk, took place on April 5–7 this year, with a return visit on April 19.
HSE said that NHS Forth Valley has developed an action plan to prioritise the requirements from the inspection.
Cathie Cowan, NHS Forth Valley chief executive, said: “This inspection took place at the beginning of April 2022 during a period of unprecedented demand combined with high levels of staff absences due to Covid-19.
“Like hospitals across the country, we had to open extra beds to create additional capacity while managing significant staff shortages.
Advertisement
Hide AdAdvertisement
Hide Ad“We recognise that the use of contingency areas is not ideal, however, local staff across the hospital continued to deliver high standards of clinical care and treatment in very challenging circumstances.
“The inspectors also highlighted the positive and caring interactions they saw between staff and patients, good team working and efforts to ensure additional staff were distributed to areas with the greatest needs.
“The majority of the report recommendations have already been addressed, in many cases on the same day of the visit, and we will ensure all are fully implemented.”
