Only three health boards hit waiting-times target
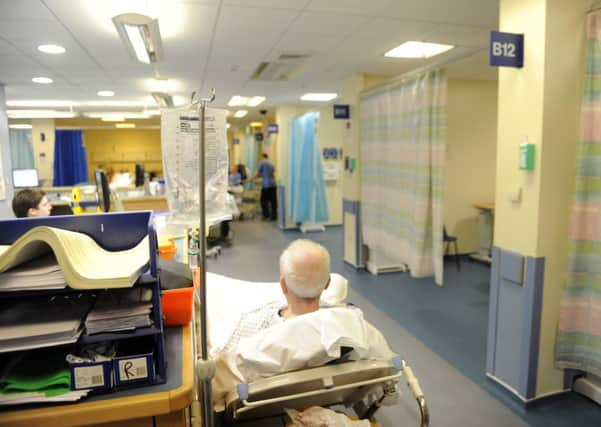

Audit Scotland found that only three boards out of 15 had consistently hit the 12-week treatment time guarantee for patients needing an operation, while the numbers waiting longer than this for an outpatient appointment almost doubled in 12 months.
The report also revealed that in some areas, large numbers of patients were having to declare themselves unavailable for treatment, extending their waits further, because they wanted to be treated locally rather than be sent further afield as boards struggled to deal with demand.
Advertisement
Hide AdAdvertisement
Hide AdAudit Scotland said the NHS and Scottish Government had improved how they managed, monitored and scrutinised waiting lists.
But the Royal College of Nursing (RCN) said the findings were a warning about the need to increase capacity to cope with growing demand.
The report – Management of Patients on NHS Waiting Lists: Audit Update – follows a previous report looking into the management of waiting times following the scandal of manipulated lists at NHS Lothian.
While it welcomed progress made by boards, Audit Scotland highlighted a number of concerns around waiting times.
Since December 2011, NHS boards have had to meet an 18-week standard from GP referral to treatment (RTT) for 90 per cent of patients. The report said 13 boards met the standard in September, although NHS Forth Valley had not achieved it since May 2012 and NHS Lothian not since September 2011.
There was less consistent progress on other targets. Since March 2010, no patient should have had to wait more than 12 weeks for their first outpatient appointment. But the report said that the ratio of people waiting over 12 weeks had increased from 3 per cent (5,993 people) in September 2012 to 5 per cent (11,544 people) in September.
In NHS Forth Valley about 20 per cent of patients (3,052 people) were on the waiting list for over 12 weeks for an outpatient appointment.
In October 2012, patients needing inpatient treatment, such as a surgical procedure, were given a legal right to receive it within 12 weeks – a target described by Audit Scotland as “challenging”. Only three boards – NHS Orkney, NHS Western Isles and the Golden Jubilee National Hospital – have achieved this each month since the guarantee was introduced.
Advertisement
Hide AdAdvertisement
Hide AdAudit Scotland said: “Auditors have highlighted the risks of NHS boards meeting increasingly demanding targets while also making increased financial savings.”
Its report in February after the manipulation of waiting lists by NHS Lothian, where patients were inappropriately classed as unavailable for treatment, highlighted concerns with the boards’ systems.
It found that the use of unavailability codes in other boards started to reduce after the problems in Lothian became public, but it was not proven why this happened.
In September 2011, 36 per cent of people waiting for inpatient treatment were classed as unavailable. But by September this year it had fallen to 18 per cent.
Theresa Fyffe, RCN Scotland director, said the report was “another serious warning shot across government’s bows” to look again at NHS capacity to meet their waiting times targets.
“All those working in our NHS know that behind all these statistics and figures are people – patients waiting to be treated in a system that’s creaking under the strain,” she said.
Health secretary Alex Neil said the report showed the progress made in improving the management of waiting lists.
Cleaning up
Significant progress has been made at a maternity hospital where inspectors had raised concerns about cleanliness, the health secretary said.
Advertisement
Hide AdAdvertisement
Hide AdAlex Neil told MSPs there had been a number of “positive quality improvements” at Aberdeen Maternity Hospital.
It comes after the Healthcare Environment Inspectorate raised “significant concerns” with the government about conditions there, following a visit in which inspectors found blood stains on some mattresses, bed rails and sinks.
Mr Neil said that he now expected NHS Grampian to “continue to ensure quality, safety and cleanliness are key priorities for all its staff”.