How do you know if you have a blood clot? Symptoms of blood clots, what causes them - and how to prevent them
The World Health Organisation (WHO) is urging countries to continue using the AstraZeneca Covid-19 vaccine as global medical leaders meet to discuss reports of blood clots.
Dr Soumya Swaminathan, WHO’s chief scientist, told a media briefing “we do not want people to panic”, as she said no association has been found so far between blood clots and Covid-19 vaccines.
Advertisement
Hide AdAdvertisement
Hide AdShe said the rates at which blood clots have occurred in people who received the AstraZeneca vaccine “are in fact less than what you would expect in the general population”.

A small number of cases of blood clots in people having the jab have been reported in Europe, prompting several countries including Germany, France, Italy, Spain, Denmark, and Norway to halt rollout of the vaccine as a precaution while investigations are carried out.
But even removed from the context of Covid-19 and vaccines, a renewed focus has been put on blood clots, with many people becoming far more aware of a condition they may otherwise have known little about.
For the hypochondriacal out there, it could be yet another thing to worry about. So what are the symptoms and signs of blood clots? How are they treated? And what should you do if you suspect you may be suffering from one?


Here is everything you need to know.
What are blood clots?
Normally, blood clots help stop bleeding when you’re injured, and are perfectly normal and safe as they plug injuries and wounds and allow them to heal properly.
But when these clots form internally or in the absence of injury, they are a worry because they can restrict the flow of blood within your blood vessels, leading to complications like stroke or heart attack.

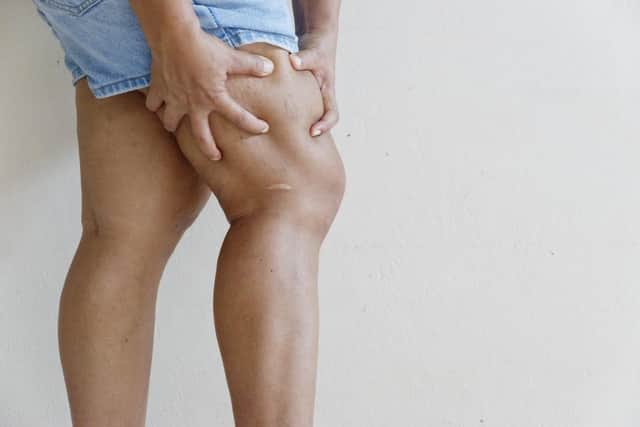
What are the symptoms of blood clots?
According to the NHS, symptoms of a blood clot include:
- throbbing or cramping pain, swelling, redness and warmth in a leg or arm
- sudden breathlessness, sharp chest pain (may be worse when you breathe in) and a cough or coughing up blood
What should you do if you think you have a blood clot?
Advertisement
Hide AdAdvertisement
Hide AdIf you are experiencing any of the above symptoms and are worried that you may have a blood clot, you should get advice from the NHS’ 111 service, either by going to 111.nhs.uk, or calling 111.
The service will be able to tell you what to do, and can arrange a phone call from a nurse or doctor if you need one.
Blood clots can be life threatening if not treated quickly, and if you are struggling to breathe or someone has passed out, you should call 999 or go to A&E.
These are symptoms of a pulmonary embolism, a blood clot in the lungs which needs to be treated immediately.
Who is most at risk from blood clots?
If you are young and healthy, you can rest assured that the chances of you suffering from a blood clot are rare. However, there are a number of factors that can increase a person’s risk of developing such a clot.
You're more likely to get them if you:
- are staying in or recently left hospital – especially if you cannot move around much (like after an operation)
- are overweight
- smoke
- are using combined hormonal contraception such as the combined pill, contraceptive patch or vaginal ring
- have had a blood clot before
- are pregnant or have just had a baby
- have an inflammatory condition such as Crohn’s disease or rheumatoid arthritis
Advertisement
Hide AdAdvertisement
Hide AdIf any of the above factors put you at an increased risk of blood clots, there are a number of things you can do to prevent them, including staying active, drinking plenty of water to avoid dehydration (and avoiding drinking lots of alcohol) and losing weight if you need to.
Those at a higher risk of blood clots can also wear flight stockings or flight socks to improve blood flow on long flights or in other situations where remaining inactive for long periods of time is unavoidable – a pharmacist can advise you about this.
For more information on blood clots, head to the NHS’ website
Is the Oxford/AstraZeneca jab safe?
Peter Openshaw, professor of experimental medicine at Imperial College London, said the decision to pause rollout of the Oxford/AstraZeneca jab could be a “disaster” for Covid-19 vaccine uptake in Europe.
Asked what he would say to those in the UK who are booked to receive an Oxford jab, Prof Openshaw told BBC Radio 4’s Today programme: “I really wouldn’t be worried at the present time.
“I think it is very clear that the benefits of being vaccinated at the moment so far outweigh the possible concern over this rather rare type of blood clot,” he added. “I think it is a disaster for the vaccination uptake in Europe, which is already on slightly unsteady ground in some countries.”
Asked why he thought the rollout pause had been taken so widely, Prof Openshaw said: “I think the committees are probably afraid of not making that decision to pause on the basis that they might be in some way thought culpable if they didn’t, but actually these are such rare events.”
Professor Anthony Harnden, deputy chairman of the Joint Committee on Vaccination and Immunisation, said there was “no demonstrable difference” in the number of blood clots seen between the general population and the 11 million who have so far received the Oxford/AstraZeneca jab to date.
Advertisement
Hide AdAdvertisement
Hide AdHe told BBC Breakfast “safety is absolutely paramount and we monitor this data very carefully,” but said “because we’re immunising so many people, we are bound to see blood clots at the same time as the vaccination.”
“That’s not because they are due to the vaccination. That’s because they occur naturally in the population. We have to remember that there are 3,000 blood clots a month on average in the general population.”
Does Covid-19 cause blood clots?
“One ought to also remember that Covid causes blood clots,” added Prof Harnden. “So, the risks of not having the Covid vaccination far outweigh the risks from the vaccinations.”
According to Johns Hopkins Medicine, some people infected with Covid-19 develop abnormal blood clotting due to the body’s “massive inflammatory response”, which can raise the prevalence of ingredients needed to form a clot in the blood.
Healthline say blood clots with Covid-19 have most often been seen in people who’ve been hospitalised with the disease, it’s still unknown how common blood clots are in individuals with mild cases, and coronavirus-related complications from blood clots can happen across all ages.