Covid Scotland: Pandemic will have 'long-lasting impact' on intensive care staff
The audit, conducted by the Scottish Intensive Care Society Audit Group (SICSAG), found intensive care units and high dependency units hugely changed by the pandemic, with demand far outstripping supply and leading to staff and equipment shortages.
Liberal Democrat health spokesperson Alex Cole-Hamilton said the audit revealed an NHS “scarred by the pandemic”. One hospital said the experience would have a “long-lasting impact” on its staff.
Advertisement
Hide AdAdvertisement
Hide AdSome units were forced to cope with three times their baseline capacity without any extra trained staff during the first wave of Covid-19.
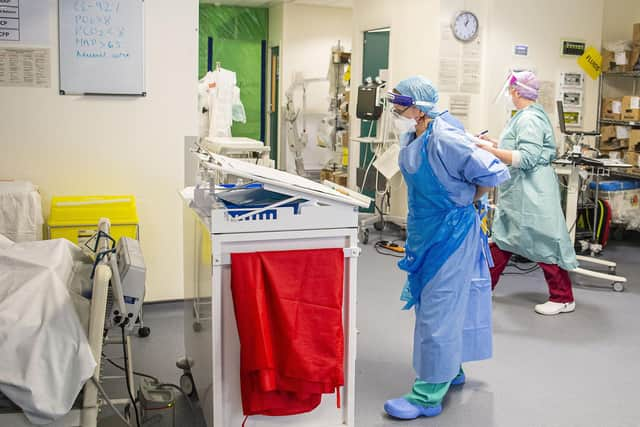

Staff shortages were “particularly challenging”, as while staff members were brought in from elsewhere they lacked ICU experience and were working with unfamiliar equipment.
Staff worked “extremely hard and in difficult conditions”, the report notes, while facing the “physical strain” of wearing PPE for long periods.
They also suffered a “significant psychological burden” in supporting dying patients while family members were not allowed to visit.
The increased strain was disproportionately felt by hospitals in deprived areas, SICSAG said, as data had shown the link between severe Covid-19 and economic deprivation.
Smaller hospitals may also have been more affected than larger ones.
University Hospital Crosshouse, in Ayrshire, was used as a unit case study in the report.
During the second wave it housed the only site for Covid critical care in Ayrshire and Arran.
Advertisement
Hide AdAdvertisement
Hide Ad"While creating additional ICU bed capacity was challenging, the additional nursing staff required to care for patients in these areas was always the greatest hurdle,” said a hospital representative.
"We relied heavily on nurses redeployed from non-ICU areas and asked them to work in ways they had never anticipated. We required our core ICU nurses to support and oversee the care given to cohorts of patients within the ICU.
"The personal impact on those individuals, who were asked to work in ways that they had never done before, was significant and will have a long-lasting impact … emotionally and physically, this experience will never be forgotten.”
The SICSAG report also reveals some high dependency units did not hit minimum standards and quality indicators in 2020, and notes high workloads due to Covid may be a factor in this.
Delayed discharges also continue to be a problem, with an estimated 8,144 days lost in 2020, the equivalent of 1,000 patient stays.
Mr Cole-Hamilton said the long-standing issues of bed blocking and staff shortages may have exacerbated problems during the pandemic.
“Staff are exhausted and many feel disillusioned,” he said.
"The mental health impacts will be long lasting. Services need more resources and staff to reduce workloads on the frontline.”
Advertisement
Hide AdAdvertisement
Hide AdThe Scottish Government labelled the report “encouraging”, as no units had unusually high death rates and standards had been met by ICUs.
“We note that some HDUs have struggled to meet these indicators and health boards have also highlighted staffing shortages in some areas,” a spokesperson said.
"Some issues remain in relation to transfer out of critical care.
“As the NHS remobilises and the Covid-related workload eases, we will continue to learn the lessons of the pandemic and work to tackle the challenges that still exist, and planned quality improvement work can resume”
A message from the Editor:
Thank you for reading this article. We're more reliant on your support than ever as the shift in consumer habits brought about by coronavirus impacts our advertisers.
If you haven't already, please consider supporting our trusted, fact-checked journalism by taking out a digital subscription.
Comments
Want to join the conversation? Please or to comment on this article.
