Hospices facing difficult decisions over limiting relatives' contact with dying patients – Dr Lewis Hughes

There’s a first time for everything but, right now, everything that is happening seems to be happening for the first time. Pictures of ICU beds show departments which have doubled or tripled capacity, busy with activity. In the sunniest April I can remember for years, the streets are eerily quiet. We’ve all seen the pictures on the news, but it isn’t just here that things are different.
Currently, I’m not on the frontline: not the Covid-19 frontline anyway. However, I am working with a team of people who really are essential, as a doctor in one of Scotland’s 16 hospices, which provide direct help to over 20,600 people every year.
Advertisement
Hide AdAdvertisement
Hide AdEven in these difficult times, hospices are looking after people with the care, kindness and humanity we associate with them. One of the best things about this is that they do it in a different way to hospitals – it’s just not as “clinical” and offers patients a more homely setting.
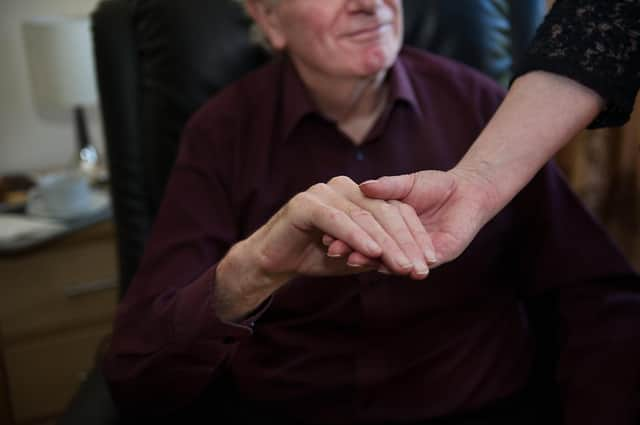
But, Covid-19 casts a long shadow; we are having to ask visitors to limit their contact with their loved ones and asking them to wear masks, aprons and gloves when they come to visit.
These difficult decisions are taken to shield patients so that coronavirus doesn’t rob them of the precious time they have left, and also to protect the staff caring for them day in, day out.
We’re so grateful to everyone who socially distances – you’re breaking the chain of infection which might otherwise find its way here.
Despite all this, the commitment and compassion of staff means our hospice is a place of joy. Eyes still wrinkle with shared laughter over the top of facemasks and meticulously washed hands are still held.
Many of our patients go home after a short spell with us, which allows us to improve symptoms to let them achieve their full potential at home.
The hospice movement began around 50 years ago and has touched innumerable lives since. Hospices are a constant at the heart of communities and have looked after generations of families.
For me, a hospice is a place where it’s truly a privilege to work. Patients and their families only get one shot at a good death and we are lucky to be able to help make it happen for them, whichever way each individual may see it.
Advertisement
Hide AdAdvertisement
Hide AdIt’s estimated that of the almost 60,000 people who die in Scotland each year, three quarters would benefit from specialist end-of-life care. With Covid-19, there’s a greater demand than ever for this, although it has been estimated that around 10,000 people per year were already missing out.
Hospice fundraising problem
Even without this crisis, there’s been a real deficit and that’s something every one of us deserves to see change. Most of us will need it eventually.
Hospices couldn’t exist without the support of local people and businesses who raise most of their funding, many are not aware that most of it doesn’t come from the NHS or the government.
Although they are one part of our journey on this earth as individuals, there is something deeply permanent and reassuringly constant about hospices.
With this crisis however, there is a question over the funding of hospices as they’ve seen retail and fundraising opportunities evaporate – charity shops can’t open and fun runs are out of the question.
Having worked in emergency departments in big cities and on remote islands, I can’t tell you how grateful NHS staff are for the kindness and gratitude they’ve been shown. Keep your local hospice in mind too when thinking about the daily heroism that continues even in these strange times. Stay safe.
Lewis Hughes is a doctor working in Ardgowan Hospice, Greenock, and co-chair of the BMA’s Scottish Junior Doctor Committee
This article has been edited as it is standard practice for some hospice patients to be sent home to be with their families after treatment and not specifically related to the risk of covonavirus
A message from the Editor:
Advertisement
Hide AdAdvertisement
Hide AdThank you for reading this article on our website. While I have your attention, I also have an important request to make of you.
With the coronavirus lockdown having a major impact on many of our advertisers - and consequently the revenue we receive - we are more reliant than ever on you taking out a digital subscription.
Subscribe to scotsman.com and enjoy unlimited access to Scottish news and information online and on our app. With a digital subscription, you can read more than 5 articles, see fewer ads, enjoy faster load times, and get access to exclusive newsletters and content. Visit www.scotsman.com/subscriptions now to sign up.
Our journalism costs money and we rely on advertising, print and digital revenues to help to support them. By supporting us, we are able to support you in providing trusted, fact-checked content for this website.
Joy Yates
Editorial Director
Comments
Want to join the conversation? Please or to comment on this article.