Clydebank hospital first to offer dedicated robotic surgery system to chest patients
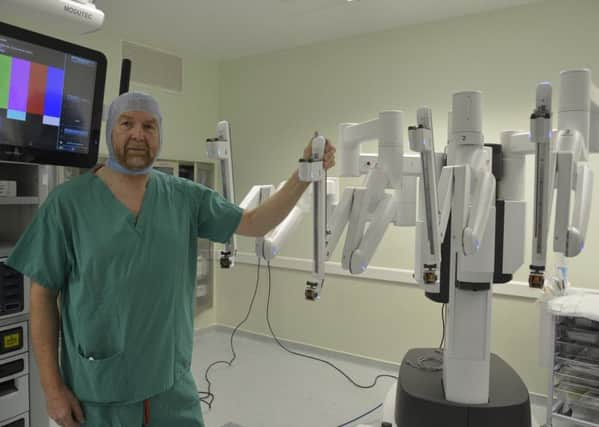

The £1.3million Da Vinci system enables surgeons to perform operations through a few small incisions, instead of more invasive procedures which take longer to heal.
While the machine has been installed at several NHS facilities across the country, the one installed at the Golden Jubilee National Hospital in Clydebank is the first to be used solely by a thoracic services unit.
Advertisement
Hide AdAdvertisement
Hide AdClinicians believe the system will pay for itself in the long term by allowing patients to return home quicker and require less care as their outcomes are improved.


Cardiothoracic consultant Alan Kirk, who has used the Da Vinci on lung patients, said: “It is probably standard of care for most urology or prostate cancer work and recently over the past five years in the UK people have diversified and started using it for chest surgery.
“We are the first unit in the whole of the UK to buy one specifically for lung surgery.
“Although it looks very complicated, it’s really an extension of what we already do on a keyhole and minimally invasive platform, but this takes things one stage further forward.
“Over the past five years, we’ve gone from big open operations for lung cancer to 80 per cent of our lung cancer procedures now being done by conventional keyhole surgery and now there is a natural extension of that, which we hope and anticipate will result in improved patient outcomes.”
Mr Kirk added his colleagues at other hospitals had to compete with various departments for access to their respective Da Vinci system.
He continued: “Our plan over the next 18 months is to develop this to the stage that those who need or want robotics will be able to get it. One of the reasons we are at this stage is that we are one of the biggest units in the UK.
“But we now have the ability to operate on more people with lung cancer – of which there are 4,600 cases in Scotland each year. Twenty years ago, only 10 per cent got an operation. Now it’s in excess of 25 per cent.”
Advertisement
Hide AdAdvertisement
Hide AdThe robotics system also benefits the surgeons who use it as well as the patients.
“The vision you get is high-definition and in 3D and is fantastic,” added Mr Kirk. “You’re looking at 360 articulation, which you cannot have working under your own hand. The precision of the surgery, the dexterity, and the vision makes it better for all.”
There are currently 38 units delivering lung cancer and chest surgery across the UK, eight of which have access to robotics.
Case study: Climbing the stairs a week after surgery is no problem for one patient
Living on the top floor of a tenement block with no lift could seem a daunting prospect for many patients recovering at home from major surgery.
But Geraldine MacAulay, 55, is already able to routinely scale the more than 80 steps to her flat in Glasgow’s leafy west end district, despite having undergone treatment in April at the Golden Jubilee National Hospital in Clydebank.
The optometrist was diagnosed that same month with adenocarcinoma, a malignant tumour formed from glandular structures in epithelial tissue.
This meant she had to undergo a lower left lobectomy, which entailed the removal of part of the lower left lobe of her lung due to cancer.
Advertisement
Hide AdAdvertisement
Hide AdSuch surgery would previously have entailed a long and often painful period of convalescence due to its invasive nature.
Instead, Geraldine is managing her recovery by simply taking four paracetamol tablets each day.
It follows surgery using a state-of-the-art Da Vinci system, which is controlled by a surgeon from a console in the operating theatre.
The hospital is the first unit in the UK to dedicate such a robotics system to lung patients within its thoracic services team.
“The diagnosis was a bolt out of the blue,” she told The Scotsman.
“It was mooted around two weeks before that my operation would be something more unusual.
“I was quite happy. I was of course pleased with anything that would give me a better outcome, and to support something progessive. Geraldine was in hospital for five nights, and was back “out and about” just a week later.
“It’s a daunting prospect having any kind of surgery as well as being diagnosed with cancer,” she continued.
“But my situation was definitely helped, despite the traumatic experience of being diagnosed, by having an easier experience (post-surgery).
“It has definitely made things better for me.”