Physiotherapy for patients suffering after knee surgery
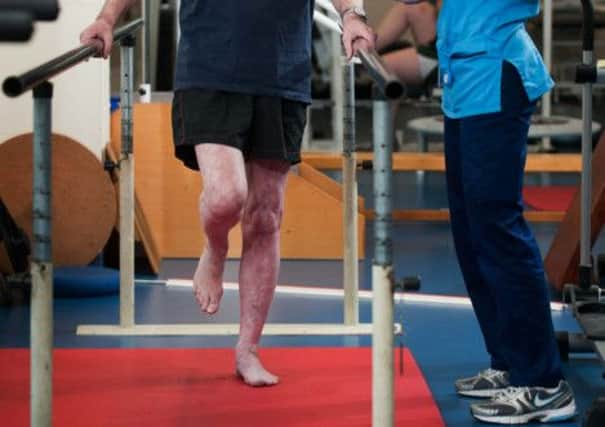

While knee replacements are one of the most effective operations carried out by the NHS, at least 20 per cent of patients may struggle to recover quickly afterwards and experience pain which seriously affects their everyday lives.
But now researchers in Scotland hope to tackle this problem by targeting intensive physiotherapy sessions at those most likely to benefit.
Advertisement
Hide AdAdvertisement
Hide AdIt is hoped this will improve the recovery of these patients, but also save the NHS money as they will need fewer appointments in the months and years after treatment.
The research, funded by charity Arthritis Research UK, has been launched as part of National Arthritis Week.
Dr David Hamilton and Professor Hamish Simpson, from Edinburgh University, and Professor Gary Macfarlane in Aberdeen, will lead the study, which will involve 440 patients across the UK.
Dr Hamilton told The Scotsman: “Knee replacement is one of the most successful forms of surgery that exists. However, patient satisfaction after surgery is not as good as after a hip replacement.
“Surveys suggest that 80 per cent of people are happy after a knee replacement, which is good but if 20 per cent aren’t happy, because we do so many operations a year, that leaves a high number of patients who aren’t happy.”
This mean around 15,000 of the 75,000-plus people in the UK who have their knees replaced each year are not completely satisfied with the result.
But Dr Hamilton said they believed there were a significant number of these people whose outcome could be improved, for example through targeting them with measures such as intensive physiotherapy sessions.
He said the key to the study was identifying the patients who would benefit most from physiotherapy, rather than giving it to everybody. While this happened for some patients at the moment, practice is not uniform across the NHS.
Advertisement
Hide AdAdvertisement
Hide Ad“For this project we are going to look at everyone six weeks after surgery to see if they are recovering quickly enough, and for the 20-25 per cent we think are recovering slowly, we will see if we can target physio to the right people to see if that makes a difference,” Dr Hamilton.
The project will also assess the effectiveness of either giving people physiotherapy exercise to do themselves at home or face-to-face sessions with a physiotherapist in the clinic over a period of six weeks.
After screening around 3,000 patients, just over 400 will be chosen to receive one of the two types of treatment,
“It makes a big difference from the cost effectiveness point of view,” Dr Hamilton said.
“But if we show that the hands on, coming into hospital physio is of benefit, then the cost-effectiveness of that will be high because if you’ve got a dissatisfied patient with persistent pain and muscle weakness you end up with lots of GP referrals, they will be on a lot of drugs and accessing a lot of health services.”
Professor Alan Silman, medical director of Arthritis Research UK, said: ”We know that for many people with arthritis, knee replacement surgery offers them a vastly improved quality of life and reduction in pain, but clearly something needs to be done for the 20 per cent who are not satisfied with the outcome.
“We are aware of the need to promote the importance of exercise and keeping moving, both for those people who have arthritis and those at risk of developing it.
“What this research will add is how best to use exercise advice and programmes to enhance the success of joint replacement surgery in people with severe osteoarthritis. This study could prove to be very significant and improve the benefits from surgery.”
CASE STUDY
Advertisement
Hide AdAdvertisement
Hide AdMichael Donnelly often found himself falling over after knee replacement surgery left his leg muscles weak and unstable.
But after taking part in intensive sessions of physiotherapy to rebuild the muscles and tissue again, he is now able to move around more easily.
The 61-year-old, from Edinburgh, had his first knee replacement in 2003, but went on to have further problems and had more surgery in 2011.
He said he believed a combination of taking part in competitive judo and working as a carpet fitter led to the damage in his knee.
Mr Donnelly’s physiotherapy involved a combination of hands-on physio in the clinic, as well as hydrotherapy exercises in a pool and also exercises at home for four months.
He also said an excellent physiotherapist had helped motivate him during the process to make sure he got the best results.
“If it hadn’t been for this effective type of physiotherapy, I would have still been going for physiotherapy,” he said.
“Now, I am without a walking stick and I am getting about quite well. I am very happy with the progress this intensive physiotherapy has allowed me to make.
Advertisement
Hide AdAdvertisement
Hide Ad“I can still have pains. But now I don’t fall over and I am more confident walking about.”
He added: “My knee was never going to be 100 per cent. But the physio has done for me what I wanted it to do.”
But Mr Donnelly said for the physiotherapy to be effective, patients had to be committed to carrying out the exercises.
“If you are of a sedentary nature then you have to be focussed and dedicated to the exercise regime,” he said.
“There might be people who would not put in the commitment that I have put in.”
Mr Donnelly said he thought the technique would work even better for someone who has had a single knee replacement, rather than the two operations he underwent,