Patients referred for ‘needless’ operations
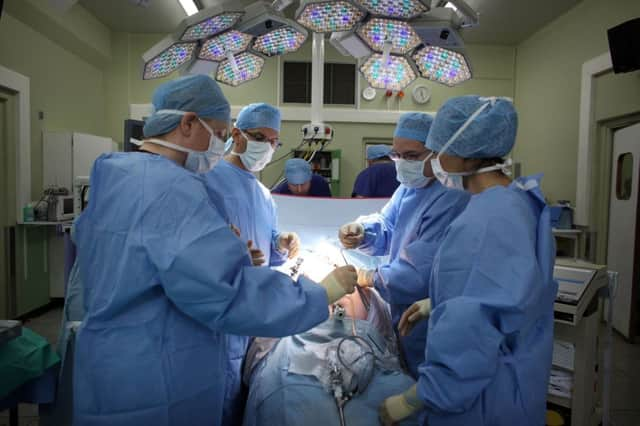

Ian Ritchie, president of the Royal College of Surgeons of Edinburgh, said emergency care had seen increasing demand in recent years as more patients turned up in A&E departments.
But, he said, to make sure surgeons could cope with the numbers being referred to them for treatment, more effort was needed to ensure they were only seeing patients who would benefit from surgery.
Advertisement
Hide AdAdvertisement
Hide AdMr Ritchie was speaking ahead of a conference on emergency care at the college in Edinburgh today. He said they were seeing more patients coming into their theatres than in the past and the meeting would debate what could be done to help cope with rising demand.
This would include making sure they were only seeing those patients who needed their help and not those referred by other departments inappropriately.
“There is this volume of work coming in,” he said. “So we need to work more closely with other disciplines to make sure that the right patients come to surgery rather than someone being allocated a complaint of, for example, an acute abdomen, and they end up on a ward and they don’t even need an operation at all.
“They need some other treatment. So that is all time- consuming to sort out. Maybe we need to work better with our colleagues in being appropriate about where people end up in the hospital. Do they need to be in the hospital at all?”
Research being presented at the conference will also touch on this problem, with claims that many referrals to specialists from GPs for patients with bone and joint issues are unnecessary.
The “costly and time-consuming” exercise of referring patients who do not need surgery, but basic physiotherapy care or pain management instead, is being tackled by the college with a course on common bone and joint problems for GPs.
Consultant trauma and orthopaedic surgeon Ali Mehdi said: “Musculoskeletal disorders are common, accounting for nearly a third of GP consultations, and this is predicted to increase as the population ages. As GPs are the first point of contact for patients, it is essential they are adequately equipped to manage this part of their workload.”
Mr Ritchie said a consequence of the increasing workload was that patients needing routine surgery may wait longer as emergency care is prioritised.
Advertisement
Hide AdAdvertisement
Hide Ad“If people have an urgent problem, we deal with it. But it does trickle down to people who have less urgent problems who find that their priority for treatment is less acute,” he said.
“In my speciality of orthopaedics, someone with a broken bone has to be fixed. However, if you have an arthritic hip and that’s really painful, because it’s not a crashing emergency you might find you are waiting a little bit longer.”
Mr Ritchie added: “Patients deciding to go to A&E with something that is not really urgent when they could wait for their GP the following day is one of the problems that does affect the A&E departments, because they have to deal with a lot of people who have a problem they think is really urgent, but it’s not that urgent and there are other ways to deal with it.”