Scotland must ‘plan for the worst’ as Omicron spreads to older population, experts warn
The Royal College of Nursing union said nurses are becoming “seriously concerned” about the safety of patients under the current pressure.
And figures from Public Health Scotland (PHS) show a 31 per cent increase in Covid hospitalisations last week, while estimating 60 per cent of patients hospitalised “with” Covid were admitted because of the virus, a similar proportion to that reported in August.
Advertisement
Hide AdAdvertisement
Hide AdSenior medics warned against dismissing patients who test positive while admitted for another condition, saying this can be a subtle distinction, especially in older people.
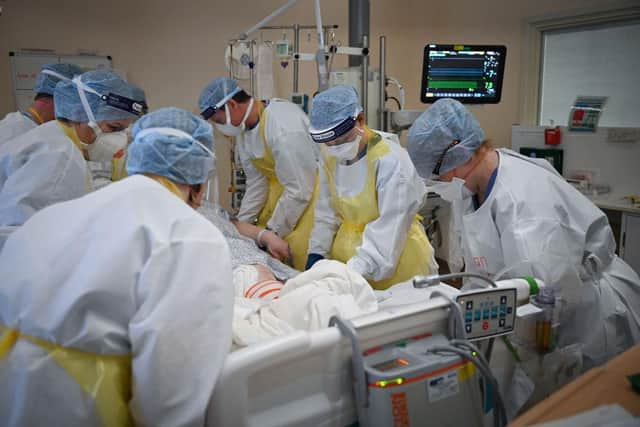

Figures show disproportionately more older people are admitted because of Covid, compared to with it, while almost half of admissions with Covid last week were those aged over 65.
Dr Antonia Ho, a clinical senior lecturer in infectious diseases at Glasgow University and consultant at Queen Elizabeth University Hospital and Monklands Hospital, warned the country must remain “cautious” as the virus spreads to older people and the return of schools potentially sparks another wave of infections.
“There are two things I'm worried about,” she said.
"There’s the fact that [Omicron] has now gone into older age groups, and we don’t really know how that will pan out … and the second point is that kids have gone back to school, and a lot of them under the age of 12 haven't been vaccinated.
"They don't have the three vaccine protection that adults have had.
“That might drive another wave … we need to plan for the worst and hope for the best.”
While many hope Scotland may be approaching the peak of cases, following around ten days behind the situation in London, Dr Ho said this view may not take account of the return of schools.
The Omicron wave is now spreading in older age groups, Dr Ho said, having been mostly an infection of young people before Christmas.
Advertisement
Hide AdAdvertisement
Hide AdWhile the majority of hospital Covid cases appear to be milder than those she was treating a year ago, Dr Ho said she was “concerned” about the proportion of older people who would end up with severe disease despite being fully vaccinated.
“We're still trying to get a feel about what hospitalised patients in the Omicron era look like,” she said.
“I would say largely that the people who are fully vaccinated, with three doses of vaccine, are not particularly unwell. My experience to date is that you're much more likely to be admitted because of Covid if you're unvaccinated or have had one or two doses of vaccine.
“But the case numbers are now just appearing in the older age groups, so it remains to be seen how that will pan out."
Professor Andrew Elder, president of the Royal College of Physicians of Edinburgh and a geriatrician, also expects to see more older patients with Covid in coming weeks.
There are currently fewer patients severely ill with Covid than in previous waves of the pandemic, he said, due to vaccination, better treatments and the apparent reduced severity of Omicron.
But he added: “It doesn't take much in a frail older person to affect them in a way that means they can no longer continue at home, and then they present to hospital.
“A level of illness from an infection that a younger person would tolerate easily, an older person may not be able to tolerate and that means they present to the hospital.”
Advertisement
Hide AdAdvertisement
Hide AdProf Elder said he hoped the current wave among younger people, which has caused significant absence among healthcare staff, would reduce before the virus spreads significantly in the older population.
He also warned against placing too much emphasis on the distinction between people hospitalised “with” and “because of” Covid.
“I can understand why there's an interest, but the difference between whether or not the patient comes to the hospital because of the virus or they’ve just got it alongside the other conditions that may be contributing to their decline is of secondary importance to the fact that more and more people are presenting to hospital,” he said.
When dealing with older patients it is often difficult to make this distinction, he said, as geriatric patients often arrive at hospital with multiple or nonspecific conditions.
Dr Ho echoed this point, saying: “I think the question is not to discount them as not a problem."
She added: “Looking at routine figures, it's not that obvious at first glance to differentiate between the two.”
Incidental Covid cases cause “equal problems” for the health service, Dr Ho added.
They need to be isolated from other patients and they increase the risk of transmission within the hospital.
Advertisement
Hide AdAdvertisement
Hide AdThe patient’s treatment for other conditions may also be delayed because of self-isolation, and those unable to return to a care home because they are infectious create extra pressure on beds and staffing.
In the week to December 28, there were 653 patients in Scotland admitted to hospital within 14 days of a positive Covid test.
In the first days of January, some 60 per cent of patients recorded as in hospital “with” Covid were admitted “because of” the virus, according to estimates from PHS based on data from NHS Greater Glasgow and Clyde and NHS Grampian.
This is a slight drop on the most recent estimate of 68 per cent, which was given in August using different methodology.
A message from the Editor:
Thank you for reading this article. We're more reliant on your support than ever as the shift in consumer habits brought about by coronavirus impacts our advertisers.
If you haven't already, please consider supporting our trusted, fact-checked journalism by taking out a digital subscription.
Comments
Want to join the conversation? Please or to comment on this article.